NMNH (reduced nicotinamide mononucleotide) is a reduced form of the popular supplement nicotinamide mononucleotide (NMN). Both molecules boost the function of NAD+ (nicotinamide adenine dinucleotide), a coenzyme that helps energize you by regulating cellular processes. NAD+ levels decline with age, leading to age-related health issues. New research suggests that NMNH could boost NAD+ levels better than NMN can. If true, NMNH supplements could be a game changer to ward off age-related health infirmities. Here's what you need to know about them.
NMNH and NMN are both supplements that help boost NAD+ levels, but there are notable differences in how they work:
| Feature | NMN | NMNH |
| NAD+ boost | Moderate increase | Nearly 10x higher increase |
| Response time | Slower | Rapid, within 15 minutes |
| Lasting impact | Short | Last up to 24 hours |
| Dosage efficiency | Higher doses needed | Minimal dose sufficient |
| Tissue impact | Limited to certain tissues | Works across multiple tissues |
| Health benefits | Basic support for aging and cells | Stronger support for cellular health and aging |
| Absorption | Standard | More efficient due to reduced form |
| Energy and metabolism | General support | Extended energy and metabolism boost |
| DNA repair | Moderate | Enhanced |
Upon ingestion, NMNH is absorbed and converted into NAD+ through the action of nicotinamide mononucleotide adenylyltransferase (NMNAT).
As NAD+ naturally decreases with age, cellular function and efficiency can decline.
Increasing NAD+ levels with NMNH helps support crucial processes like energy metabolism, DNA repair, and cellular maintenance.
This increase in NAD+ can help mitigate age-related declines in cellular function, promoting healthier aging at the cellular level.
NMNH is being studied for its ability to combat age-related decline, showing potential benefits at both cellular and systemic levels, such as:
While NMNH supplements are generally considered safe for most individuals, some may experience side effects, including:
NMNH should also be used cautiously by individuals with certain medical conditions, such as:
Note: Before starting NMNH, it's advisable to check with a healthcare provider, especially if you have any health conditions.
Nicotinamide riboside (NR) and NMNH are NAD+ precursors, yet they vary in chemical structure, metabolic pathways, and physiological effects.
Upon ingestion, the enzyme nicotinamide riboside kinase converts it into NMN, which then enters the NAD+ biosynthesis pathway.
It can be directly used in the NAD+ biosynthesis pathway without converting to NMN.
A 2021 study highlights that NMNH is more effective than NMN in boosting NAD+ levels.
Lab tests and studies on mice showed that NMNH increased NAD+ levels more efficiently in both cases.
Additionally, NMNH increased NADH, the reduced form of NAD+, which is essential for cell energy production.
It also impacted metabolism by slowing down key energy pathways, such as glucose breakdown and the citric acid cycle, to improve cellular health.
In lab experiments, NMNH caused cell cycle arrest and inhibited cell growth, while no significant change in mouse weight was observed.
While both NMN and NMNH enhance NAD+ levels, NMNH's effects may offer superior benefits for health and aging.
The FDA has banned NMN under the "drug exclusion clause" of the Federal Food, Drug, and Cosmetic Act (FD&C Act).
According to section 201(ff)(3)(B) of the Act, any substance classified as an approved drug or tested as a new drug cannot be marketed as a dietary supplement.
Since NMN underwent clinical investigations before being sold as a supplement, the FDA determined it didn't qualify as a dietary supplement and banned it in the U.S. market.
Should You Take DGL Supplements For Treating Acid Reflux?
Are Postbiotics Better Than Probiotics For Gut Health?
https://www.uthpeak.com/blog/what-is-nmnh-matter-for-your-health
https://www.uthpeak.com/nmnh-vs-nmn
https://downloads.regulations.gov/FDA-2023-S-0023-0084/attachment_1.pdf
https://www.healthline.com/health/nmn-nicotinamide-mononucleotide-benefits-side-effects-and-dosage
https://pmc.ncbi.nlm.nih.gov/articles/PMC6145238
https://pmc.ncbi.nlm.nih.gov/articles/PMC7384296
https://pubmed.ncbi.nlm.nih.gov/33793246
https://www.fda.gov/media/131878/download
Experiencing bloating and tiredness after meals? Does your stomach ache, or do you find it hard to concentrate after eating certain foods? There might be a hidden cause – lectins. Though found in many healthy foods, lectins can cause problems for some people, like tummy troubles, skin issues, and feeling worn out. Keep reading to learn about lectins, which foods have lots of them, signs to watch for, and most importantly – what you can do if they're making you feel unwell. If you want to take charge of your health and feel better, this article gives simple tips and useful information about dealing with lectins.
Did You Know?
Certain gene changes can make you prone to food intolerance and drug allergies. These genes are mostly involved in immune system regulation, and changes in them may result in the immune system attacking some components in the food. You can use your ancestry genetic testing data to uncover this information. Learn more.
Lectin intolerance is a food sensitivity that occurs when certain people react badly to foods with lots of lectins.
Lectins are proteins in plants like beans, grains, fruits, and vegetables. They stick to carbohydrates in our guts, messing with how we absorb nutrients and causing digestive discomfort.
Lectins are stable in acidic environments, which is a protective feature for plants. However, this means that it is not easily broken down in the gut.
Hence, while lectins may be fine for most people, some might experience adverse reactions or other symptoms after consuming them.
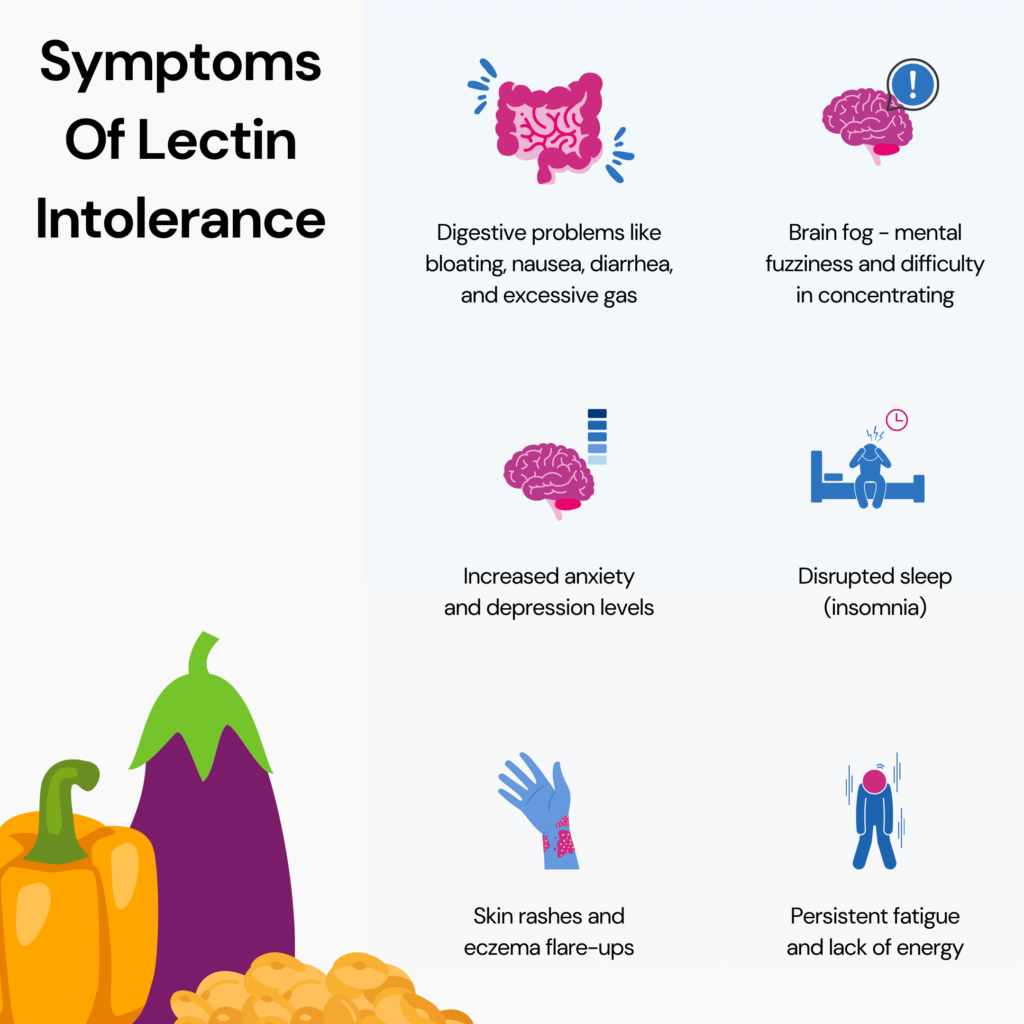
Lectin intolerance can cause various symptoms, highlighting the significant impact on overall health and well-being.
Several commonly consumed foods have high levels of lectins. Here are 6 examples:
Adding to the list of foods already mentioned above as high in lectins, here are some more examples:
Understanding what might increase the risk of lectin intolerance is crucial for managing symptoms. Here are some potential factors:
The specific genes associated with lectin sensitivity are still being studied, but two genes might be involved:
Remember, lectin sensitivity involves many genes and other factors, and research is still ongoing to understand it better.
Bananas contain moderate lectins, but they are mostly harmless, called agglutinins. The human gut does not readily absorb these agglutinins, and they do not cause significant health problems for most people.
While coffee does contain lectins, the amount is generally considered low and not thought to be harmful to most people. Some studies suggest that coffee may have some health benefits, like lowering the risk of neurodegenerative diseases and type 2 diabetes.
There is no known way to flush lectins out of your body. Here's why:
Lectins do not negatively impact everyone. While some people may develop symptoms after eating lectin-containing foods, others can tolerate them without issue.
It's important to note that responses vary on an individual basis. Testing your sensitivity to lectins is essential.
Additionally, foods with lectins offer health benefits like antioxidants, stabilized insulin, and blood sugar regulation.
Research shows populations eating diets high in lectin-rich legumes, whole grains, and nuts have lower rates of cardiovascular disease and type 2 diabetes.
So, while lectins can cause problems for some, they also provide benefits.
It's best to consult a professional to determine if you can incorporate lectin-rich foods in moderation as part of an overall balanced approach.
Managing lectin intolerance involves alleviating symptoms rather than curing the underlying condition.
As many reported symptoms involve gastrointestinal distress, reducing or eliminating high-lectin foods from one's diet may provide relief.
Restricting the consumption of foods that worsen symptoms under a healthcare professional's instructions can help manage discomfort.
The goal is to identify and minimize the consumption of specific high-lectin foods that cause symptoms in each individual.
This personalized approach helps tune into the body's signals, control flare-ups, and improve overall wellness.
Reducing lectin intake can help alleviate discomfort for those sensitive to these compounds.
Here are some straightforward ways to lower your lectin consumption:
Note: It's best to consult a healthcare provider for personalized guidance, considering your health history and symptoms.
Lectin intolerance can cause digestive issues, fatigue, and brain fog in some individuals.
While lectins are found in various healthy foods, they can trigger reactions in sensitive individuals.
These plant proteins can bind to gut carbohydrates, potentially impacting nutrient absorption and causing discomfort.
Bloating, nausea, diarrhea, brain fog, anxiety, fatigue, skin issues, and disrupted sleep are potential signs of lectin intolerance.
Examples of high-lectin foods include red kidney beans, soybeans, wheat, peanuts, tomatoes, potatoes, and others.
Frequent antibiotic use, gut imbalances, leaky gut, plant-based diets high in lectins, and certain genes might increase the risk.
To reduce lectins, you can boil, soak, sprout, or choose processed beans. Depending on your sensitivity, you may also need to adjust your diet.
https://www.hsph.harvard.edu/nutritionsource/anti-nutrients/lectins/
https://www.healthline.com/nutrition/foods-high-in-lectins
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10084985/
https://www.healthline.com/nutrition/dietary-lectins
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5960708/
https://pubmed.ncbi.nlm.nih.gov/21892520/
https://www.ncbi.nlm.nih.gov/books/NBK5968/
https://pubmed.ncbi.nlm.nih.gov/11030554/
https://pubmed.ncbi.nlm.nih.gov/29590460/
In an ever-changing world, what if we told you there was technology that could analyze an individual’s gut biology and gain insights into their health? The friendly bacteria in your gut can help strengthen immunity and influence cognitive abilities. Gut bacteria also affect your risk for certain brain diseases, such as Alzheimer’s disease, Parkinson’s disease, and autism. That’s what Viome, a health testing company in the United States, has set out to develop! Let's take a look at Viome reviews, highlighting what the internet has to say about them, and add our own two cents.
Viome is a health health testing company that uses mRNA (mitochondrial RNA) samples to identify the microbes in an individual’s gut.
With an in-depth gut microbiome analysis, the company allows individuals to identify their risk for chronic diseases and other health concerns, such as cancer and aging.
Viome offers personalized recommendations for nutrition, supplements, and precision therapeutics based on the test results.
The company's headquarters is in Washington, United States.
Most companies that offer microbiome testing use a person’s stool sample.
There are two types of fecal testing that a company may offer–
Here’s what a typical microbial testing looks like:
Viome uses AI and RNA sequencing to identify and quantify microbes.
These techniques can study various strains of viruses, bacteria, yeast species, and other parasites.
Viome test analyses how microbes function and the metabolites they produce.
The results are then used to control an individual’s gut microbiome and reduce the risk for chronic diseases.
The company claims to do this by offering food, lifestyle, and supplement recommendations tailored to an individual’s needs based on their test results.
Viome offers the following products:
A person provides blood or stool samples for this test to analyze their gut microbiome and gene expression.
The scores help individuals measure their stress, immune response, and mitochondrial and cellular health.
These scores also determine the person’s biological age and if it is the same as their chronological age.
This test requires a stool sample to assess gut microbiome health.
The individual receives a dietary recommendation chart with foods and supplements that they can benefit from and help optimize their gut health.
Based on test results, each individual receives a personalized and precise recommendation for supplements, including vitamins, food extracts, minerals, herbs, and probiotics.
These nutrients are formulated on demand and can be shipped directly to the individual every month.
Viome’s personalized probiotic and prebiotic formulas promote microbial richness and diversity, supporting gut health and total body wellness.
Viome offers a one-time purchase of tests and also allows plans on a subscription.
The subscription plans may include probiotic and prebiotic supplements and annual tests.
Once you book your test or subscribe to the annual plan, follow the instructions and send the required samples to the lab.
The test results will be available around four weeks after the lab receives the samples.
You can see your results online on the company website or the app.
Viome performs their test analyses at a CLIA-certified US laboratory in Bothell, WA.
The lab is certified to meet certain quality standards and ensure the accuracy and reliability of results.
There have been a few negative reviews about Viome due to the delayed test results.
Though many people have positively reviewed how a Viome test result has improved their health, more research is required to prove this.
Let’s dive deep into reviews and reports about how Viome may improve health.
Since all the authors of the above studies were employees of Viome and the company sponsored these studies, there is bias, and the results may not be reliable.
Our Take: While some studies have highlighted the effectiveness of Viome tests, these are limited in both quantity and scale. Substantial clinical research and validation will be needed before Viome can reliably support individuals in transforming their gut health and reducing their risk for chronic conditions.
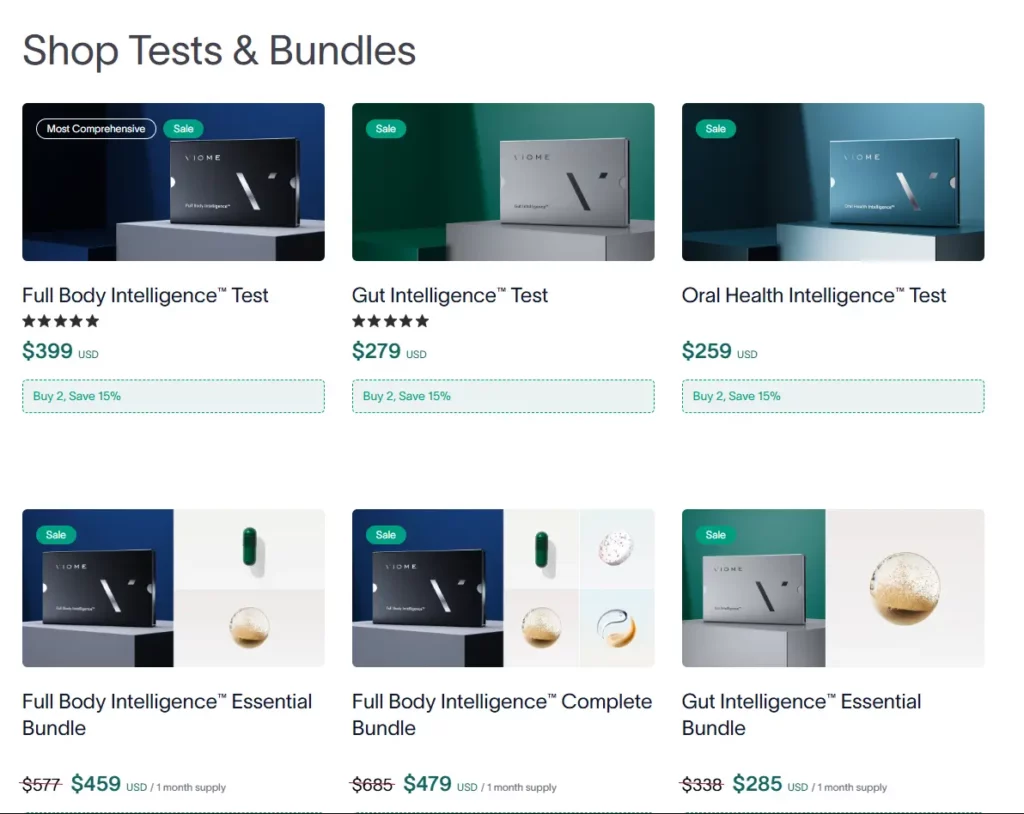
The pricing of different Viome tests is given below:
| Type of Test | Price (in USD) |
| Full Body Health Solutions | $169.15/month |
| Full Body Intelligence Test (Test Only) | $299 |
| Gut Health Solutions | $67.15/month |
| Gut Intelligence Test (Test Only) | $279 |
| Oral Health Solutions | $67.15/month |
| Oral Health Intelligence Test (Test Only) | $259 |
| Precision Supplements | $126.65/month |
| VRx My·Biotics™ Gut Formula | $67.15/month |
| VRx My·Biotics™ Toothpaste & Gel | $67.15/month |
| CancerDetect Test for Oral and Throat Cancer | $599 |
There are several pros and cons that you must consider before opting to undergo a Viome test.
The Better Business Bureau has not accredited Viome.
However, it has given Viome an A+ rating.
The company has also resolved 52 complaints over the last 3 years.
However, the company scored 1.24 out of 5 stars from 59 customer reviews.
People who reported improvement in conditions such as irritable bowel syndrome and chronic obstructive pulmonary disease gave positive reviews.
Most negative reviews highlighted the following reasons:
While Viome has mixed reviews on Reddit, most people were unhappy with the company’s test, processing time, and results.
There is speculation that Viome themselves have pushed artificial positive reviews on Reddit.
Some customers are unhappy with the “unscientific” nature of the test results.
Some individuals have stated that their Viome test helped them better understand their body and gut health.
The affordability of Viome tests works in favor of the company as well.
The primary difference between Viome and EverlyWell is that Viome provides personalized dietary recommendations based on gut microbiome analysis.
Everlywell, on the other hand, provides general recommendations for improving gut health.
Since Viome offers personalized recommendations, they may be more effective in improving gut health.
Viome tests are not FDA-approved and, therefore, are not recommended for diagnosis of conditions.
However, Viome recently received an FDA Breakthrough Device Designation for its saliva tool, which can help screen for oral cancers.
After the lab receives the sample, it may take around 4 weeks for the results to become available online- on the company website or the app.
Here are a four few things to keep in mind before taking a Viome test:

Genetic Lifehacks Review: What You Should Know Before Buying

10X Health System Reviews: Detailed Overview, Cost, Pros & Cons

Genomelink Traits And Reports: A Comprehensive Review
The curly girl method took the internet by storm and became a much-needed blessing for all those flaunting their gorgeous curls. It has helped enhance the look of the natural curls for many. But the hair products are definitely not the roots of curly hair. Your hair texture is predominantly genetic, and the curly hair gene is more dominant than the straight hair gene.
Understanding your hair type helps explain how genetics influence your locks. Hair is commonly categorized using the Andre Walker Hair Typing System, which ranges from Type 1 (straight) to Type 4 (coily). Here's a simple breakdown:
| Different Types Of Hair Patterns | |
| Type 1: Straight Hair Straight hair is smooth and lacks any natural curl or wave. It's known for its sleek appearance and ability to reflect light, giving it a shiny look. | |
| 1A | Very straight and fine, with little volume or body |
| 1B | Straight but with more texture and medium thickness |
| 1C | Straight with coarse strands, prone to slight waves and frizz |
| Type 2: Wavy Hair Wavy hair sits between straight and curly hair types. It has an "S" shape and can range from loose, subtle waves to more defined ones. | |
| 2A | Soft, loose waves with a fine texture |
| 2B | Defined "S"-shaped waves, more prone to frizz |
| 2C | Deep waves nearing curls, thick and resilient hair |
| Type 3: Curly Hair Curly hair forms distinct loops and spirals. The curls can vary from loose rings to tight corkscrews. | |
| 3A | Large, loose curls about the size of sidewalk chalk |
| 3B | Bouncy ringlets similar in size to a marker |
| 3C | Tight curls the diameter of a pencil, voluminous and springy |
| Type 4: Coily Hair Coily hair, also known as kinky or afro-textured hair, features tight curls in a zigzag pattern. The strands are densely packed and can shrink significantly when dry due to the tight curl pattern. | |
| 4A | Dense, spring-like coils about the size of a crochet needle |
| 4B | Z-shaped coils with sharp angles and less defined patterns |
| 4C | Tightly coiled with minimal definition, highly prone to shrinkage |
Genetics plays a crucial role in determining various characteristics of your hair. Here are some key aspects influenced by your genetic makeup:
The shape of your hair follicles—determined by genetics—largely dictates whether your hair is straight, wavy, curly, or coily. Round follicles produce straight hair, while oval or twisted follicles result in wavy or curly hair.
Natural hair color depends on the type and amount of melanin pigments. Genes influence whether you have more eumelanin (leading to black or brown hair) or pheomelanin (resulting in red or blonde hair).
Genetic factors determine the thickness of individual hair strands and the overall density of hair follicles on your scalp.
The rate at which your hair grows and its maximum potential length are genetically predetermined. Genes influence the duration of the anagen (growth) phase of the hair cycle, affecting how long your hair can grow.
Conditions like androgenetic alopecia (male or female pattern baldness) are influenced by genetics. Specific genes can make hair follicles more sensitive to hormones like dihydrotestosterone (DHT), leading to gradual hair thinning and loss.
The onset of graying is also genetically controlled. Genes affect the decline in melanin production over time, which causes hair to lose its color and turn gray or white.
Yes, curly hair is genetic - however, there’s no one single gene responsible for it.
The genetics behind hair curliness is complex and multifactorial.
Several genes have been implicated in determining hair texture, but a prominent one that has been studied in relation to hair curliness is the TCHH (trichohyalin) gene.
The protein produced by the TCHH gene plays a role in the development of the hair shaft.
It is localized in the inner root sheath of hair follicles.
Variations or differences in this gene have been associated with the difference in hair curliness across populations.
A 2009 study identified a genetic variant in the TCHH gene that is responsible for 6% of the variance in curly, wavy, and straight hair.
However, it's essential to understand that the presence or absence of this variant doesn't guarantee straight or curly hair but rather influences the odds.
Other genes like EDAR and FGFR2 have also been linked to hair texture.
The interplay between multiple genes, each with its variants, determines the final hair phenotype, making the genetics of hair curliness a complex trait.
Curly hair, from a genetic standpoint, tends to be a dominant trait.
Dominant traits are those that overpower recessive ones. Dominant traits need only a single copy from either biological parent to be expressed.
On the other hand, recessive traits need two copies, one from each biological parent, to be expressed.
Straight hair is a recessive trait.
However, like many genetic traits, hair type isn’t a straightforward dominant or recessive game.
If both parents have a combination of genes (one for straight and one for curly hair), their offspring can exhibit a range of hair textures.
Even within families with a strong prevalence of curly hair, hair type could vary significantly, emphasizing the complex interplay of genes.
Did You Know?
Not just hair, but many aspects of your skin, from the risk for premature wrinkles and acne to your ideal skincare routine, are influenced heavily by your genes! Your ancestry test DNA data includes 700,000 markers, which can be used to learn in-depth about your skin aging and skin health. This report will help you understand your skin requirements better and aid in graceful aging. Learn more.
Some reports say that less than 20% of the world’s population have proper curly hair, making it rarer than straight or wavy hair.
The hair spectrum includes rare types like Type 1c (straight and thick) and Type 4c (tight coils with zigs and zags).
The prevalence of these types varies by ethnicity and region.
Genetics lays the foundation, but environment and lifestyle choices build upon it.
Hormonal changes, nutritional choices, stress, and even hair care routines can shift hair texture over time.
For instance, prolonged exposure to humidity or salty water can influence hair’s texture.
Prolonged heat treatments or chemical applications can lead to a permanent change in hair type.
Additionally, hormonal fluctuations, especially during pregnancy or menopause, can lead to hair texture modifications.
While genetics favor curly hair offspring, if one or both parents possess curly hair, it isn’t absolute.
Genes can sometimes skip generations.
So, even if your parents do not have curly hair if someone in the previous generations did, there’s a chance of you having curly hair.
Both parents contribute genes, so neither parent singularly determines curly hair.
It’s the combination of genes from both that paints the final picture.
Absolutely. The mystery of genetics means that if both parents carry the recessive curly hair gene, their child could very well sport a curly mane.
Naturally, curly hair is relatively common but varies by population and ethnicity.
Globally, it's estimated that about 11% of people have naturally curly hair.
The prevalence can be higher or lower in specific regions due to genetic diversity and ancestral backgrounds.
Curly hair is found across all ethnicities, though its prevalence and type can vary.
It is common among people of African descent, who often have tightly coiled hair.
Wavy and curly hair types are also prevalent in Middle Eastern, European, South Asian, and Latin American populations due to diverse genetic backgrounds.
Our hair's texture, whether curly or straight, often prompts the question: "Is hair type genetic?" Delving into the science behind our locks reveals that genes, such as TCHH, play a crucial role in shaping our hair's form, confirming that curly hair is genetic. While genetics typically suggests that curly traits tend to dominate, it's not the sole influencer. Environment and lifestyle choices weave into the narrative, adding depth to the story of every curl and strand.
https://pubmed.ncbi.nlm.nih.gov/5173315/
https://journals.plos.org/plosgenetics/article?id=10.1371/journal.pgen.1006594
https://medlineplus.gov/genetics/gene/tchh/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2775823/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7432488/
If you’ll believe it, one simple fruit could add a refreshing flavor to your tea and potentially transform your health! Bergamot, a citrus fruit, has quietly earned its place in the world of natural remedies. Its traditional roots and enviable nutrition profile make it an excellent candidate for cholesterol management. But what makes this fruit so unique? Can it seamlessly integrate into modern wellness? Let’s uncover the exceptional properties of this fruit and learn whether you should try bergamot for cholesterol management.
Bergamot, also called Citrus bergamia, is a citrus fruit with a yellow color and a size similar to an orange.
The name "bergamot" is believed to have originated from the Italian city of Bergamo, where the fruit was first commercially traded.
Traditional Italian medicine has utilized bergamot peel and its juice for centuries, valued for their healing properties.
The fruit is also famous for adding its distinctive flavor to Earl Grey tea.
Bergamot is rich in natural compounds such as flavonoids and phytochemicals and is believed to offer a range of health benefits.
It’s commonly available as supplements, essential oils, juices, and extracts.
Additionally, its calming aroma is often enjoyed through inhalable sticks designed for therapeutic purposes.
This fruit is valued for its uses in health, aromatherapy, and even tea-making.
Bergamot's precise source remains debatable, but its cultivation is concentrated in several key regions.
Bergamot is rich in polyphenols, a diverse group of natural compounds vital in regulating fat and sugar metabolism.
These include various flavonoids, such as
and flavones, such as
They lower total cholesterol, triglycerides, and LDL ("bad") cholesterol while improving insulin sensitivity and regulating communication between fat tissue and the body.
When combined with pectins and vitamin C in supplements, bergamot polyphenols enhance the production of adiponectin, a hormone that regulates metabolism.
They also help balance the appetite hormones leptin and ghrelin.
This process aligns with the lipostat theory, which proposes a system for maintaining body fat levels.
Bergamot polyphenols have a dose-dependent effect, meaning their impact increases with the amount consumed.
They also work with statins (cholesterol-lowering medications), helping improve the lipid profile and support cardiovascular health.
Bergamot holds significant potential for improving overall health, impacting the body and mind. Here are a few of its key benefits:
Bergamot may help lower cholesterol levels based on several studies.
In a 2018 study, researchers looked at how bergamot extracts affected people with high cholesterol and other related health issues. They divided the participants into three groups: one received a placebo (no active ingredient), one received a standard bergamot extract (BPF), and the last group received a special form of the extract (BPF Phyto).
Here’s what they found:
The placebo group did not show any changes.
Both forms of bergamot were effective in lowering cholesterol and blood sugar levels within just 30 days, and there was no significant difference between the two types of extracts in how well they worked.
In summary, bergamot appears to be beneficial for managing cholesterol levels and improving overall health.
A review of 12 studies found that bergamot supplementation contributed to significant reductions in cholesterol levels:
These outcomes from the studies highlight bergamot’s potential to reduce cholesterol and triglycerides across various lipid categories.
Bergamot supplementation has been shown to lower cholesterol levels, with clinical trials observing reductions throughout 1 to 6 months of consistent use.
While some individuals may experience changes within several weeks, the exact timeframe can vary.
This variation depends on factors such as overall health, initial cholesterol levels, and adherence to the recommended dosage.
There's no single "best" form of bergamot for cholesterol reduction.
Various forms have been studied, including bergamot fruit extracts (widely used in research), standardized supplements with specific bergamot polyphenols, and juice.
While each has shown potential in clinical trials, further comparative studies could help verify these promising claims.
The dosage of bergamot for managing cholesterol can vary based on the form (extract, oil, or supplement), concentration, and individual health.
Studies suggest that daily doses of bergamot extract generally fall between 150 mg and 1500 mg.
Bergamot is typically safe, but one should be cautious of its possible side effects, especially when consumed in large amounts or misused.
Here are some potential side effects:
It’s best to avoid bergamot for cholesterol management if you fall into these categories:
No, bergamot is not hard on the liver when used correctly. A randomized controlled trial showed that people taking a supplement with bergamot had a 48.2% reduction in liver fat compared to 26.9% in the placebo group.
These results suggest that bergamot can improve liver health when used in the right amounts.
Bergamot has shown potential kidney-protective effects in studies.
Bergamot juice helped reduce malondialdehyde (MDA) levels in rats on a high-fat diet, indicating a decrease in oxidative stress.
Kidney tissue examination also suggested that bergamot juice prevented kidney damage caused by high cholesterol.
However, more research is needed to understand its effects on human kidneys fully.
Bergamot can be a versatile addition to your diet, bringing flavor and potential health benefits.
Below are practical ways to include it in your meals:
Consult a medical professional before starting, stopping, or continuing a supplement regimen.
Adults may take bergamot extract in doses of up to 1000 mg daily for 4 to 12 weeks.
Consult a healthcare professional regarding the ideal dosage for your specific condition.
Depending on your preference and body response, you can take bergamot in the morning or night.
Some find it helps promote calmness during the day, while others prefer it at night for its relaxing properties.
Observe how it affects you and choose the time that best suits your needs.
Earl Grey tea contains bergamot, but whether the concentration can influence cholesterol levels is unclear.
Bergamot and black tea might aid digestion and help lower blood pressure and cholesterol, which benefits heart health.
However, further studies are required to confirm the impact of bergamot in Earl Grey.
Managing cholesterol naturally often involves a combination of strategies. Here are some key lifestyle and dietary changes to consider:
Bergamot has shown some cholesterol-lowering effects, but it works differently from statins.
While statins reduce cholesterol by inhibiting the HMGCR enzyme, bergamot does not directly affect this enzyme.
Instead, it may lower cholesterol by affecting cholesterol synthesis and absorption.
Although bergamot shows potential, it should not replace statins, especially for individuals who need strong cholesterol management.
Always consult a healthcare provider before considering bergamot as an alternative to statins.
It's difficult to definitively say which is the best because "best" depends on individual needs and circumstances.
Many natural supplements are available that may help lower cholesterol, but their effectiveness and potential side effects vary.
Discuss any new supplement with your physician before use, especially if you have underlying health problems or are taking other medications.
Both berberine and bergamot are great for cholesterol management, but bergamot is especially effective at lowering LDL and improving HDL for better overall cholesterol levels.
It is an excellent choice if your main focus is improving your cholesterol profile.
Berberine also helps with cholesterol and is especially good for your gut and digestion. It aids in keeping gut bacteria balanced and promotes better digestion.
Berberine is also known for its ability to control blood sugar, making it ideal for supporting both blood sugar and digestive health.

Fluctuating Cholesterol Levels And Alzheimer's Risk - The ApoE Connection

Lima Beans: Nutrition Facts, Health Benefits, Side Effects, & More

Can Weekend Naps Improve Your Heart Health?
https://www.medicalnewstoday.com/articles/bergamot-supplement-benefits
https://www.health.com/health-benefits-of-earl-grey-8598609
https://www.mdpi.com/2673-8392/1/1/16
https://pmc.ncbi.nlm.nih.gov/articles/PMC8569986
https://pubmed.ncbi.nlm.nih.gov/10940328
https://www.nhs.uk/conditions/statins
https://pmc.ncbi.nlm.nih.gov/articles/PMC6392855
https://pubmed.ncbi.nlm.nih.gov/28591067
https://www.mayoclinic.org/diseases-conditions/schizophrenia/symptoms-causes/syc-20354443
https://pubmed.ncbi.nlm.nih.gov/32379683
https://pmc.ncbi.nlm.nih.gov/articles/PMC6497409
https://www.tandfonline.com/doi/full/10.1080/10408398.2019.1677554
https://www.healthline.com/health/cholesterol/can-bergamot-lower-cholesterol
https://www.sciencedirect.com/topics/medicine-and-dentistry/furocoumarin
https://www.medicalnewstoday.com/articles/325113
https://www.medicalnewstoday.com/articles/brisk-walking
https://pmc.ncbi.nlm.nih.gov/articles/PMC8469228
https://pmc.ncbi.nlm.nih.gov/articles/PMC7431622
https://www.health.com/condition/cholesterol/cholesterol-lowering-supplements-what-works-what-doesnt
https://pubmed.ncbi.nlm.nih.gov/19655295
https://www.sciencedirect.com/topics/medicine-and-dentistry/malonaldehyde
https://www.webmd.com/vitamins/ai/ingredientmono-142/bergamot
https://botanicalinstitute.org/citrus-bergamot-vs-berberine
As someone who can devour a plate of buffalo wings without breaking a sweat, I often find myself puzzled by my friends' reactions to spicy food. While I enjoy the spicy kick, they’re left gasping for water, tears streaming down their faces. This stark contrast sparked my curiosity about what really determines our spice tolerance. After diving into some fascinating research, I discovered that our ability to handle heat isn’t just about taste preferences—it has a significant genetic component!
The taste buds present on our tongue can taste salty, sweet, or sour foods.
However, there are no receptors to taste spicy food.
Therefore, the heat you feel from spicy food is a pain sensation.
Chilli peppers have a component called Capsaicin that makes them hot and spicy.
This component binds with a receptor called TRPV1 on the tongue, giving a heat sensation.
This receptor is involved in regulating your body temperature.
Repeated exposure can gradually make this receptor less sensitive.
Spice tolerance has a lot to do with genes.
In fact, a study has reported that up to 58% of differences in spice tolerance among individuals can be attributed to genetics.
While there may not be a single gene contributing to spice tolerance, it is hypothesized that people with higher tolerance have fewer TRPV1 receptors on the tongue.
This means that they may be less sensitive to the burning and painful feeling of spice and can thus enjoy it more.
However, the good news is that spice tolerance is something that can be built with repeated exposure.
When you consume spicy foods regularly, you desensitize the receptors which will allow you to enjoy them without the burning sensation.
Spice tolerance might have a surprising connection with personality.
People who are thrill seekers and are more adventurous might like spicy food.
People who take more risks and enjoy otherwise scary situations like an extreme roller coaster ride might like spicy food.
People who love spicy food and don't find it painful have fewer Capsaicin receptors.
It is not that they cannot taste the spiciness altogether, but they feel less pain and heat.
Over time, eating spicy food can desensitize nerve endings, resulting in a higher spice tolerance.
People from Mexico, Korea, or India are naturally more tolerant of spicy food because they consume them regularly.
They have become desensitized to the pain from a young age.
Building your spice tolerance is not only possible but can also be an enjoyable journey! Here are some effective strategies to help you gradually increase your ability to handle spicy foods:
Begin by incorporating small amounts of spicy ingredients into your meals.
This could be as simple as adding a pinch of chili flakes to your pizza or a dash of hot sauce to your soup.
The key is to start with a level of spiciness that is manageable for you and slowly increase it over time.
Regularly consuming spicy foods can help desensitize your TRPV1 receptors.
The more frequently you expose your taste buds to spice, the more accustomed they will become.
Over time, this repeated exposure can lead to a higher tolerance, allowing you to enjoy spicier dishes without discomfort.
Combining spicy elements with familiar flavors can make the transition easier.
For instance, try mixing spicy salsa with guacamole or adding chili powder to a dish you already love.
This way, you can enjoy the flavor of spice without overwhelming your palate.
Not all spicy foods are created equal.
Some spices provide heat without intense burning sensations.
For example, try milder peppers like poblano or Anaheim before tackling hotter varieties like jalapeños or habaneros.
This variety can help you find a comfortable entry point into the world of spice.
When consuming spicy foods, have dairy products like yogurt or milk on hand (not recommended if you are lactose intolerant).
Dairy contains casein, which binds to capsaicin and helps neutralize its effects.
Staying hydrated is also essential, as it can alleviate some of the discomfort associated with eating spicy foods.
According to a recent report by Technomic, Asians appear to have the highest spice tolerance, while Caucasians, have the least.
It is a mix of both nature and nurture. Some may be born with fewer spice receptors in their tongue, which makes them less sensitive to the burning sensation of spice. Repeated exposure to spice right from a young age can also build up spice tolerance.
A 2014 study revealed that higher salivary testosterone levels were associated with higher consumption of hot sauce and lower self-reported perception of spiciness. However, more research needs to be done to check if this theory has any merit.
Spice tolerance is mainly genetic.
Capsaicin, the spice component found in chili peppers, can elicit pain when binding to the TRPV1 receptors.
People who have fewer TRPV1 receptors are less sensitive to spicy food.
Spice tolerance also has a lot to do with someone's personality.
Spice tolerance can be gradually built by eating small amounts of spicy foods over time.
http://www.sciencedirect.com/science/article/pii/S0031938412003095

How Genes Influences The Tendency To Prefer Bitter Foods?

How Nutrigenomics is Changing the Way We Think About Food