Imagine a world where doctors prevent diseases before they start, rewrite faulty genes, and customize medications to your DNA. This isn’t science fiction—it’s the future of genetic testing. Genetic testing is transforming how we understand ourselves, unlocking the secrets of our DNA. From detecting inherited diseases to personalizing treatments, it’s reshaping healthcare. As science advances, we must navigate its promises, possibilities, and ethical dilemmas too.
From basic biological tools to advanced genetic sequencing, human identification has come a long way.
Before DNA testing, scientists relied on methods like blood typing and serological testing, which could indicate relationships but lacked precision.
The evolution of DNA analysis has transformed forensic science, paternity testing, and ancestry research.
Early methods: Blood typing, serological analysis, and HLA testing (1920s–1970s)
The NGS revolution (2010s- present)
Next-generation sequencing (NGS) has revolutionized DNA testing, enabling high-precision sequencing and expanding its applications.
A key development made possible by NGS is a safer, more straightforward alternative to paternity testing.
Non-invasive prenatal paternity (NIPP) testing can analyze a maternal blood sample as early as 7 weeks into pregnancy.
Currently, DNA testing is extensively employed in various fields, including forensics and paternity testing.
It helps solve criminal cases by matching DNA evidence from crime scenes to suspects.
In paternity cases, it helps confirm biological relationships between fathers and children.
Beyond forensics, DNA testing is used in medical areas like bone marrow and organ transplants.
It helps doctors check if a transplant is successful and if the body accepts the new cells or organs.
DNA tests can also identify the origin of tumors after a transplant, determining whether they are from the donor or the recipient.
DNA testing uses advanced techniques like PCR (to make copies of DNA), DNA sequencing (to determine the exact sequence), and STR analysis (to create unique DNA profiles).
These methods enable accurate and efficient DNA analysis for various applications. The article also discusses the several technologies involved.
DNA testing accuracy today is remarkably high, reaching up to 99.99%.
The accuracy depends on the number and quality of genetic markers analyzed during the test.
Technological advances have also improved DNA testing’s ability to work with smaller or degraded samples while maintaining high precision.
A DNA test looks at your genetic makeup to identify changes in your genes, chromosomes, and proteins. It helps detect genetic conditions or risks, such as:
The decision to take a DNA test is personal and should be discussed with a genetic counselor or geneticist, as it has both benefits and limitations.
DNA testing is becoming more accessible, with varying costs depending on the type of test and purpose:
Ongoing developments in DNA testing are enhancing capabilities in health, ancestry, and forensic science, with the latest techniques outlined below:
Karyotyping analyzes chromosome number and structure, while FISH uses fluorescent probes to identify specific DNA sequences.
It examines all chromosomes simultaneously, detecting changes smaller than those identified by karyotyping or FISH.
The future of genetic testing looks very promising and is set to change how we treat medical conditions.
With ongoing advancements, genetic testing will soon replace traditional methods of prognosis prediction, enabling more precise and personalized treatment plans.
One of the most exciting possibilities is creating customized treatments for patients who are most likely to benefit, reducing unnecessary therapies and improving results.
As technology advances, genetic testing will help detect more disorders and give us a better understanding of complex diseases, like various forms of cancer.
Researchers are also progressing in mapping genetic variations that could provide crucial insights for future therapies.
This progress will help guide the next generation of clinical research, offering hope for more effective solutions and improved patient care.
DNA testing is constantly evolving, and it’s important to match this pace.
Accessibility is the key to meaningful innovation, and this is where Xcode shines.
Xcode is currently able to accurately and comprehensively analyze genetic data from over 50 raw DNA data providers.
We deliver some of the most affordable DNA reports on the market within just 24 hours of ordering.
Xcode’s blog is regularly updated with informative, engaging articles on the latest scientific trends.
This reflects our dedication to innovation as well as universal accessibility in the field of genetic testing.
The adoption of genetic testing has significantly increased, particularly over the last two decades.
The number of genetic tests registered in the United States has grown dramatically, with 129,624 tests listed as of November 2022.
Globally, the number is even higher, reaching 197,779 tests.
This growth is primarily driven by clinical tests, with over 90% of tests used for diagnostic purposes.
The number of new genetic tests made available yearly has also grown, from 607 new tests in the US in 2012 to 3,097 in 2022.
On a global scale, new genetic tests grew from 1,081 in 2012 to 6,214 in 2022.
Most of these tests aim to diagnose conditions rather than research, demonstrating the growing role of genetic testing in healthcare.
Even though genetic testing holds significant value for understanding genetic conditions, many people choose to decline.
The following are some key reasons why:
We are making significant progress towards gene editing, with CRISPR-Cas9 technology leading the way.
This system enables scientists to edit DNA with great accuracy, and it has already been applied to plants, animals, and human cells in research.
The ability to use gene editing to eliminate or treat genetic diseases, such as sickle cell anemia and cystic fibrosis, is within reach.
Right now, gene editing is mainly used for research, but there is potential for it to be used in clinical treatments in the future.
Specifically, it could prevent genetic disorders from being passed to future generations.
While gene editing is not yet a routine part of medical treatments, its rapid development suggests it could soon play a key role in fighting genetic diseases.

3 Ways DNA Testing Can Improve Your Health And Wellness
Genetic Markers Explained

Genes vs. Lifestyle: Striking The Right Balance
https://dnacenter.com/history-of-dna-testing
https://pmc.ncbi.nlm.nih.gov/articles/PMC1200713
https://www.nature.com/scitable/topicpage/paternity-testing-blood-types-and-dna-374
https://medlineplus.gov/genetics/understanding/testing/genetictesting
https://dnacenter.com/blog/how-much-does-a-dna-test-cost
https://pmc.ncbi.nlm.nih.gov/articles/PMC10376292
https://cellandbioscience.biomedcentral.com/articles/10.1186/s13578-019-0314-y
https://www.sciencedirect.com/science/article/abs/pii/S0379073819302014
https://medlineplus.gov/genetics/understanding/genomicresearch/snp
https://pmc.ncbi.nlm.nih.gov/articles/PMC6976916
https://www.mdpi.com/2227-9040/6/4/43
https://pmc.ncbi.nlm.nih.gov/articles/PMC6240714
https://www.nature.com/articles/s41551-021-00760-7
https://www.testing.com/genetic-testing-techniques/
https://pmc.ncbi.nlm.nih.gov/articles/PMC10142561
https://pmc.ncbi.nlm.nih.gov/articles/PMC6119550
https://pmc.ncbi.nlm.nih.gov/articles/PMC5524257
DNA testing is rapidly changing the way we approach our health. It provides deep insights into our genetic makeup, opening doors to understanding risks for conditions like heart disease, diabetes, and cancer, long before symptoms emerge. Research suggests that 80% of chronic diseases are preventable with the proper knowledge and lifestyle changes. What if DNA testing could provide the exact information needed to personalize your health strategies? The potential benefits are vast, from enhancing your diet to managing mental health. Keep reading to discover three ways DNA testing can improve your health.
The healthcare system faces several key limitations that affect patient care.
Here are some of the significant challenges:
DNA testing provides essential information in several areas, from health to family connections, making it a vital tool for addressing key issues today, such as:
DNA testing has evolved beyond ancestry research and is now a valuable tool for improving health.
Here are three ways DNA testing can enhance your health:
DNA testing reveals how your body processes nutrients, reacts to specific foods, and metabolizes fats, carbs, and proteins.
For example, it may show if you're predisposed to lactose intolerance, gluten sensitivity, or how you metabolize caffeine.
This information allows you to adjust your diet to meet your body's needs, leading to better digestion, energy, and overall health.
DNA tests highlight your genetic risk for conditions like heart disease, diabetes, or certain cancers.
While these results don't guarantee you'll develop these conditions, they enable you to take proactive measures.
For instance, if you're more prone to heart disease, exercising regularly, eating a heart-healthy diet, and scheduling routine check-ups can be practical steps.
DNA testing provides valuable information on genetic factors that affect mental health.
Some tests analyze genes associated with conditions like depression, anxiety, or ADHD.
Knowing your genetic predisposition helps develop a personalized mental health plan with therapy, lifestyle changes, or treatments.
Note: Always consult a doctor to interpret your DNA test results and create a personalized health plan based on your genetic profile.
DNA testing is now considered highly accurate, with reputable companies reporting reliability rates exceeding 99.9%.
Despite this accuracy, privacy remains a significant concern, as genetic data may be vulnerable to unauthorized access if not securely stored after submission.
Even with security measures like encryption, your genetic information remains vulnerable.
It could be shared without your consent with entities like research institutions or pharmaceutical companies.
Protecting your privacy can involve choosing providers with strong data privacy policies, being mindful of how your data is utilized, and minimizing data sharing.
Since genetic data cannot be changed like a password, users must carefully consider the long-term implications before undergoing DNA testing.
You can get a DNA test from several places:
The rising cost of healthcare is a big concern for people, governments, and employers.
Expensive treatments, medicines, and administrative costs make it harder to afford care and increase health inequalities.
One primary reason for these high costs is inefficiency in healthcare systems.
Many tasks, such as insurance claims, patient billing, and record management, still require manual work. This slows things down and raises expenses.
Additionally, healthcare relies on unstructured data, which makes it challenging to analyze and use information appropriately.
These inefficiencies worsen other problems, such as limited access to care, managing long-term illnesses, and meeting the needs of an aging population.
DNA testing has several downsides, including:
According to a systematic review, whole-exome sequencing (WES) costs between $555 and $5,169, while whole-genome sequencing (WGS) costs between $1,906 and $24,810.
These estimates vary based on laboratory fees, sequencing depth, data interpretation, and whether clinical consultations are included.
The review also found that many cost analyses lack transparency, making it unclear which components are covered.
While WES and WGS can potentially improve genetic diagnosis, more research is needed to evaluate their cost-effectiveness in clinical practice.
While genetic tests provide valuable insights, they do not offer a complete picture of health or future risks.
They mainly identify common genetic variations but may miss rare ones contributing to certain conditions.
Genetic testing cannot detect diseases influenced by environmental factors, infections, or random events.
These tests also cannot confirm whether someone will develop symptoms of a disorder, how severe it will be, or how it may progress.
Additionally, many genetic disorders have no effective treatment, even if identified.

Genetic Markers Explained

What Are RSIDs?

Genes vs. Lifestyle: Striking The Right Balance
https://pubmed.ncbi.nlm.nih.gov/28523941
https://www.ncbi.nlm.nih.gov/books/NBK221522
https://www.apollohospitals.com/diagnostics-investigations/dna-test
https://www.nhlbi.nih.gov/health/cystic-fibrosis
https://www.mayoclinic.org/diseases-conditions/tay-sachs-disease/symptoms-causes/syc-20378190
https://www.bda.uk.com/resource/dietary-dna-tests-how-they-work-and-what-theyre-useful-for.html
https://www.hudsonalpha.org/understanding-genetic-risk-how-genetics-shape-your-health
https://pmc.ncbi.nlm.nih.gov/articles/PMC9840515
https://www.cdc.gov/adhd/about/index.html
https://www.kff.org/health-costs/issue-brief/americans-challenges-with-health-care-costs/
https://www.nature.com/articles/gim2017247
https://medlineplus.gov/genetics/understanding/testing/riskslimitations
https://my.clevelandclinic.org/health/diseases/21751-genetic-disorders
In a room of 25 people, chances are, only two people are likely to be left-handers. Handedness is the preference for one hand over the other for everyday tasks like eating or writing. There are three types of handedness – Left-handedness, right-handedness, and mixed-handedness (an equal preference for either hand). Data collection studies say that about 12% of the world’s population is left-handed, and about 1% is mixed-handed. Biologically, handedness could have a link to the coordination and function of your brain's right and left hemispheres. This article will explore the genetics behind handedness and why there are so many more right-handers than left-handers.
Handedness refers to an individual’s preference to use one hand (called the dominant hand) over the other for tasks like writing, eating, cutting with scissors, etc.
Globally, more than 85% of people are right-handed.
Left-handedness is a fairly rare trait with a prevalence of under 15%.
Mixed-handedness is defined as preferring different hands for different tasks, and ambidextrousness is the ability to perform tasks equally well with either hand.
The widespread prevalence of right-handedness suggests that it could be beneficial but also begs the question of how left-handedness originated.
Typically, the left and right hemispheres of the brain handle different activities.
For example, the left hemisphere is the language center and is responsible for formulating grammar and vocabulary.
The right hemisphere is involved more with visual processing and spatial sense.
Michael Corballis, PhD, a psychologist at the University of Auckland in New Zealand and a brain hemisphere specialist, mentioned to APA - “There's an advantage to cerebral dominance because it localizes function to one hemisphere; otherwise, information has to cross back and forth across the corpus callosum, and that can sometimes cause problems."
It is suggested that during early development, small variations—due to genetics, hormones, or even random "developmental noise"—can influence how the brain organizes itself.
For some people, these variations lead to a preference for using the left hand.
Twin and family studies suggest that genetics plays a role in handedness.
They report that up to 40 genes could lead to handedness through common genetic influence.
Their effect on handedness is cumulative; no single gene decides handedness.
Each of these genes exerts a small and weak influence, but together play a big role in hand preference.
Scientists have only identified a few of these genes.
One gene of interest is NME7 (NME/NM23 Family Member 7).
This gene regulates the position of organs along the left/right axis of the body.
It likely plays a role in body symmetry and your tendency to prefer your left hand.
Left-handedness persists as a minority trait in human populations due to a combination of genetic, neurological, evolutionary, and cultural factors.
Left-handedness has links to increased risks for some health conditions.
However, the strength of evidence and validity of some findings remain dubious.
Here are some key findings from scientific studies:
Inflammatory bowel disease: Left-handers have a 2x higher risk of developing Crohn’s disease or ulcerative colitis.
Cardiovascular disorders (CVD): A 2023 study by the Medical College of Georgia reported that vascular endothelial function and heart rate variability are lower in southpaws than in right-handers. This supports the increased risk of CVD in left-handers.
Breast cancer: Postmenopausal left-handed women have a higher incidence, possibly linked to prenatal estrogen exposure.
Recommended for you: Can Your Dominant Hand Affect Your Grip Strength?
Two right-handed parents could have a left-handed child if they are both carriers of the left-handed gene without expressing it themselves. They could pass on one allele each to their child.
Within a year, at about 10-11 months, infants develop a preference for one hand over the other. This preference stabilizes over the next year or so.
A 2019 study reported no significant difference in the IQ of left- and right-handed individuals in a population.

Is Curly Hair Genetic? How DNA Affects Your Hair Type

Is Height Genetic?
Are Cavities Genetic? The Root Cause
Imagine you're visiting a friend in a new city. They tell you, "My house is just a few blocks from Central Park." You may not know the exact address, but knowing Central Park's location makes your search much easier. Genetic markers are biological landmarks on the map of our DNA. Scientists know the precise location of these markers on our chromosomes. This knowledge allows them to explore the surrounding genetic neighborhoods to pinpoint specific genes associated with diseases, ancestry, or how our bodies interact with medications.
Genetic markers are specific DNA sequences with well-defined locations on chromosomes that assist in identifying variations within genes or entire genomes.
The genetic marker may constitute a gene portion or possess no known function.
The primary objective of genetic marker typing is determining which gene variations are present at specific locations on your DNA.
Some common examples of genetic markers include:
Let's go over them one by one.
Single nucleotide polymorphisms (SNPs) are variations in a single nucleotide base at a specific location in the DNA sequence.

Restriction fragment length polymorphisms (RFLPs) are variations in DNA fragment lengths caused by differences in restriction enzyme cut sites.
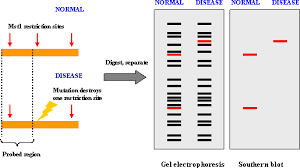
Variable number of tandem repeats (VNTRs) are repeating DNA sequences where the number of repeats varies among individuals.
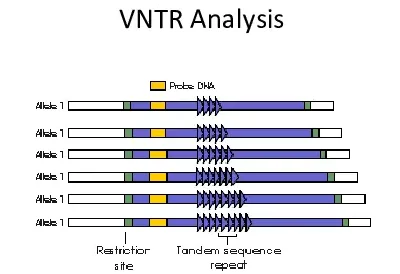
Copy number variants (CNVs) refer to differences in the number of copies of a particular DNA segment found in different individuals.
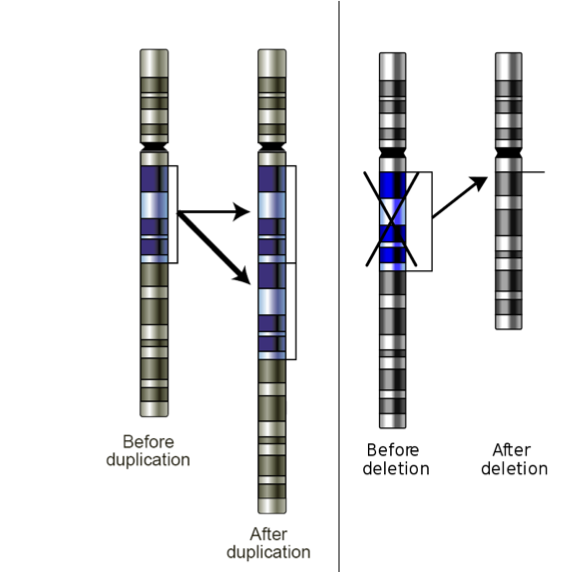
Short Tandem Repeats (STRs) are repeating DNA sequences that exhibit variable numbers of repeats among individuals.
However, these are not the only types of markers; various other forms of genetic markers exist, and scientists are constantly discovering newer types.
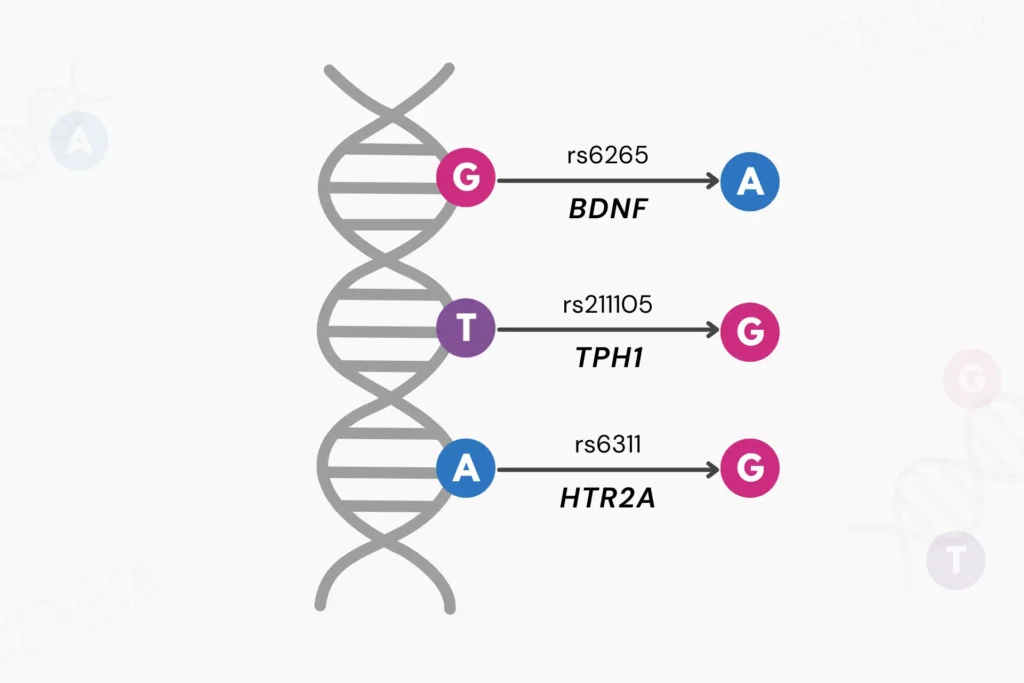
An RSID (Reference SNP-cluster IDentification) is a distinctive identifier designated for single nucleotide polymorphisms (SNPs) within the dbSNP database.
Moreover, they identify short nucleotide insertions, deletions, and short tandem repeats.
Researchers and databases employ RSIDs to monitor and analyze genetic variations.
RSIDs follow the format "rs##"—for example, rs429358 links to Alzheimer’s risk.
Genetic markers influence traits by altering gene function or regulation. It’s essential to understand that most traits are polygenic; this means they are affected by multiple genes and numerous genetic markers.
A single marker rarely dictates a trait.
The combination of markers inherited from both parents creates a unique genetic profile that contributes to a trait's overall expression.
This genetic influence extends across various aspects of life, from physical traits like hair and eye color to health predispositions and wellness traits.
Genetic markers also play a crucial role in ancestry tracing and paternity testing, helping us understand our roots and biological relationships.
Hair Color: A gene called MC1R produces pigments in the body that regulate our skin, hair, and eye color. Research has identified a variant in the gene named rs1805007 linked to a higher chance of developing red hair.
Lactose Intolerance: We're born with the ability to digest lactose but lose it with time due to a variation in the gene that produces lactase, which digests lactose. While the extent of it varies, the variant changes the genes, which leads to little or no lactase enzyme production.
Body weight: We humans share the same basic genetic makeup; however, gene variations can influence individual traits, including body weight. Specific gene variants can affect metabolism, appetite regulation, and how the body stores fat, predisposing some individuals to weight gain or obesity.
Physical Performance: Genetic factors also influence endurance and other athletic abilities. Specific gene variants may contribute to greater aerobic capacity, muscle efficiency, and recovery, potentially enhancing an individual's endurance levels.
Several gene variants have links to improved physical strength and performance, including ACTN3, PPARA, and AMPD1.
These variants influence muscle fiber composition, energy metabolism, and recovery efficiency.
Genetic testing helps assess disease risks and personalize healthcare, but markers only indicate susceptibility, not certainty. Environment and lifestyle also play a significant role in health outcomes.
Cancer: While lifestyle and environmental factors play a significant role, certain genetic markers can indicate a higher susceptibility to specific cancers. For instance, BRCA1 and BRCA2 markers signal a higher risk of developing breast cancer and ovarian cancer.
Drug Response: Our bodies process medications differently; genetic markers can reveal these variations. Specific gene variants can affect how effectively our bodies metabolize certain drugs, influencing their efficacy and potential side effects.
For example, variations in the CYP2C19 gene can alter how the body processes certain antidepressants, allowing healthcare providers to tailor prescriptions for optimal treatment outcomes.
Markers are key in tracing genetic lineage and verifying biological relationships.
Ancestry Tests: Genetic markers are used to trace ancestral origins and migration patterns. Specific markers can reveal a person's ethnic background and geographic origins, connecting them to populations around the world. For instance, a marker on chromosome 15 might link someone to Indigenous American heritage, providing a deeper understanding of their ancestral roots.
Paternity Tests: Genetic markers, specifically Short Tandem Repeats (STRs), are used in paternity tests to confirm biological relationships accurately. These markers are highly variable between individuals, making them ideal for identifying parent-child relationships.
For example, DYS391 on the Y chromosome helps confirm biological parentage with high accuracy, offering clarity in questions of lineage.
Genetic markers function as essential indicators of genetic variations and can offer valuable insights into an individual's health and disease risk; however, they possess limitations.
Three categories of DNA markers exist: autosomal, paternal, and maternal.
Autosomal markers: These unique DNA sequences, scattered across the genome and not sex-specific, assess overall ancestry.
Paternal (Y-DNA) markers: Located on the Y-chromosome, fathers pass these markers down to their sons. Y-DNA markers trace paternal lineages.
Maternal (mtDNA) markers: These DNA markers, located in the mitochondria, are inherited from the mother. Mitochondrial DNA markers trace maternal lineages.
Siblings share approximately 50% of their genetic markers (inherited randomly from their parents). However, this percentage can fluctuate due to various factors. Although the genetic contribution is significant, it is essential to remember that siblings are still distinct individuals. This uniqueness arises because of the random assortment of genes during reproduction.
Yes, offspring can inherit genetic markers from their parents via Mendelian inheritance.
That’s why families often share traits like height or diabetes risk.
Genetic markers play a crucial role in diagnosing numerous diseases or assessing the risk of their development.
Diagnostic Testing: A specific genetic marker can definitively confirm a diagnosis in certain cases. For example, a particular mutation in the CFTR gene confirms cystic fibrosis.
Risk Assessment: Genetic markers commonly assess disease risk. They can indicate an elevated risk for a disease but do not guarantee that an individual will develop the condition. Environmental factors, lifestyle choices, and other genes significantly influence disease development.
Some diseases for which genetic markers are used include:
What Are RSIDs?

Genetic Methylation Test In 2025: The Where, How, & Why

How Genes Influence Your Risk For Lactose Intolerance
https://humangenetics.medicine.uiowa.edu/resources/how-does-genetic-testing-work
https://www.genome.gov/genetics-glossary/Genetic-Marker
https://my.clevelandclinic.org/health/diagnostics/23065-dna-test--genetic-testing
https://medlineplus.gov/genetics/understanding/testing/riskslimitations
https://www.nature.com/articles/ng.3716
As the scientific community continues to unlock the mysteries of the human body, more and more people are turning to DNA tests to learn about their health and ancestry. While the price of a DNA test can vary depending on the type of test and the company you choose, this guide will give you an idea of how much you can expect to pay for a DNA test.
The cost of DNA tests varies widely based on the type. Ancestry tests typically range from $59 to $119, with MyHeritage offering the cheapest option at around $36. Health and wellness assessments cost between $100 and $640, with Xcode Life providing reports starting at $30. Paternity tests range from $130 to $200 for at-home options and $300 to $500 for legal tests. Molecular genetic tests can vary from $100 to $2000 depending on complexity. Overall, prices reflect a broad spectrum depending on the specific test and provider.
Depending on the type and complexity, a DNA test price may vary between $99 to more than $2000.
In some cases, additional testing may be required, increasing the cost.
In some states, insurance covers a portion of certain types of genetic tests.
From the date of sample collection, the results may be ready within a few days to a few weeks.
The turnaround time is much quicker if the genetic test is crucial for timely diagnosis (such as prenatal tests).
Different types of genetic tests investigate different things and are priced accordingly.
Let’s have a look at some important types of genetic tests.
| Type of Test | Average Cost |
| Ancestry Test (direct-to-consumer) | $59-$119 |
| Health and Wellness Assessment (direct-to-consumer) | $100-$640 Xcode Life’s Special Price: starting from $30 |
| Paternity Test | At home: $130-$200 Legal: $300-$500 |
| Molecular Genetic Tests | $100-$2000 |
Genetic ancestry tests, also called genealogy tests, aim to analyze the shared genetic regions between individuals to establish their relationship.
Ancestry testing allows one to learn their ethnicity and information about their ancestors.
It is the cheapest DNA testing option with most companies and can range from as low as $59 to around $119.
*as of 02nd Feb 2025
Also Read: How To Login To AncestryDNA + Health Reports At 55% Off!
Genetic tests can now help healthcare professionals and other consumers understand the risk of developing a health condition.
This enables personalized preventive measures and optimal treatment.
Further, owing to the rising popularity of nutritional supplements, genetic companies are introducing lifestyle and wellness tests (such as nutrition or fitness genetic tests) to promote better health.
Most companies price these tests at $100 to $600.
Many companies also combine health and ancestry tests and price them around $200.
Did You Know? You can use your existing DNA data from ancestry genetic tests to get Xcode Life's reports within 24 hours!
DNA paternity tests are one of the most common types of DNA tests.
The individual and the alleged father get a genetic test, and a specialist compares the shared DNA regions between them to establish paternity.
At-home DNA paternity tests cost around $130-$200, and legal paternity tests can cost up to $500.
Molecular tests are mostly used for diagnostic purposes.
They look for abnormal changes in one or more genes
Molecular genetic tests employ DNA sequencing, a process that determines the order of the 4 letters (A, T, G, and C) in the human genetic code.
Costs vary depending on the type of test: single variant, targeted gene, gene panel, whole-exome, and whole-genome.
| Company | Average Test Cost** |
| Xcode Life (DNA kit not provided) | Single tests: $30-$50 Bundles: $110-$149 (850 traits) (Ongoing sale: $69 - $99) |
| 23andMe | $99-$999 |
| AncestryDNA | $99-$199 |
| MyHeritage DNA | $89 (sale price $36) |
| Family Tree DNA | $79 - $449 |
| Living DNA | $124-$225 (sale price $90-$169) + shipping |
| Genomelink | $39-$199 |
| SelfDecode | $318-$417 (with optional add-ons ranging from $49-$249) |
| CircleDNA | HK2,299-HK2,499 |
| Nebula Genomics | $249-$899 |
Some direct-to-consumer companies, like Sequencing, offer free services that allow you to upload your existing DNA data to get some basic information for free.
Many insurance plans cover most clinical genetic tests recommended by physicians. However, direct-to-consumer tests have poor insurance coverage, and only a few companies/insurance plans offer reimbursement.
Dog tests help the owners know the specific breeds to allow better care.
Despite the rising popularity of dog DNA testing, only a few companies offer quality services.
The tests can cost anywhere from $60 to $200, based on the knowledge you’re seeking and how deep you want the analysis to be.
Pregnancy DNA tests cost depending on the nature of the test.
The most common types of pregnancy tests include
The cost of a full DNA test, or a whole-genome sequencing test, can vary widely, ranging from $400 to over $1,000, depending on the depth of analysis and the provider.
Some research studies offer free DNA testing if you qualify as a participant, but free consumer testing options are rare and usually limited.
The results can also be too technical and difficult to interpret and understand.
Insurance may cover genetic testing if it is deemed medically necessary, such as for hereditary disease screening, but typically not for recreational or ancestry tests.
Genetic testing can be highly valuable for those seeking insights into health risks, ancestry, or personalized wellness.
Tests for specific hereditary conditions can help with early intervention and personalized health strategies.
However, it is important to understand the difference between clinical and consumer genetic testing.
If you are looking for a diagnosis or a confirmatory yes or no, clinical testing should be your choice.
If your goal is to optimize your health based on certain genetic tendencies, consumer genetic testing can be a very useful tool.
DNA testing has potential drawbacks, such as privacy concerns over data storage and sharing.
Unexpected results can also reveal sensitive information, such as unknown family relationships or health risks, which may be emotionally challenging.
Some tests can be costly, and insurance coverage is generally limited to medically necessary genetic tests, not personal interest or recreational tests.
Further, improper interpretation of results or following recommendations in the report without doctor consultation can harm your health.
Yes, direct-to-consumer companies allow individuals to order their own genetic tests for health, wellness, or ancestry without needing a doctor’s referral.
The pricing of DNA tests varies depending on the type, use, and the company offering the genetic test.
Basic ancestry tests cost around $99, while health and wellness ones can cost as much as $450.
Molecular diagnostic tests can cost anywhere from $100-$1000.
We often talk about being "well," but what does that mean? Do we just mean not being sick? Or is there something more to it than that? Many people mix up the ideas of "health" and "wellness," but they're different. Health is like your body's physical condition – are you disease-free? Wellness is a much bigger picture. It's about your overall well-being, including your physical health, mental and emotional health, social connections, and how you feel about your life. When we understand the little differences between health and wellness, we can make better choices that help us feel good in every way, not just physically. It gives us more control over how we live and how happy we are.
The World Health Organisation (WHO) defines health as "a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity."
This means that health is not simply the absence of illness.
Good health encompasses physical fitness, mental stability, and everyday societal interactions.
It is a holistic state that allows individuals to live a fulfilling life.
WHO defines wellness as "the optimal state of health for individuals and groups."
Wellness is the active pursuit of good health and a meaningful life.
It encompasses actions and behavior that help you reach your fullest potential.
The two elements of health are:
Wellness is an idea that focuses on a broad spectrum of different elements.
The 12 elements of wellness are:
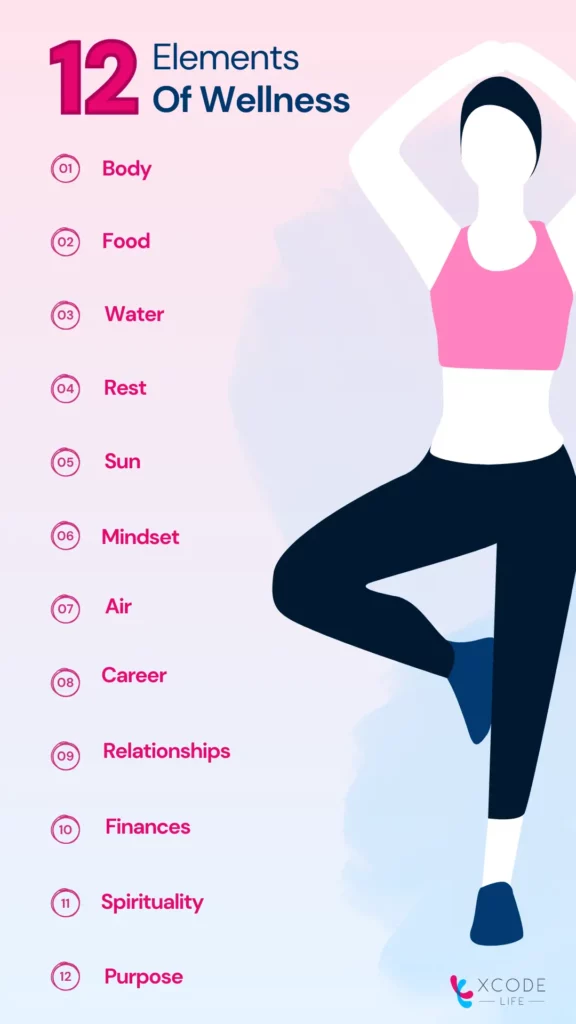
The main difference between health and wellness is the active process of achieving health, which is the goal.
Health is your predisposition to developing certain diseases like type 1 diabetes, hypertension, or cardiovascular diseases.
Wellness is the daily choices you make, like eating a balanced and taking the time out for exercise.
While you cannot always choose health, you can actively pursue wellness.
Here is a comparison between health and wellness:
Well-being is a state of equilibrium or balance in life.
It can be affected by life changes, personal problems, family responsibilities, etc.
Some define well-being as prosperity, happiness, comfort, and good health.
However, these descriptions might not fully describe well-being.
Well-being is more of a personal description of how an individual feels.
Wellness is more intricately connected to your physical and mental health.
In general, wellness practices aim to achieve optimum health through mindful practices and choices in life.
On the other hand, well-being is more connected to your emotional state.
Someone can be extremely ill yet described to be content and happy.
Similarly, someone can be physically and mentally healthy yet not feel balance and fulfillment.
This is the difference between wellness and well-being.
We recommend the Genome Pack! Rated 4.7/5 By Users Like You
This report is not a diagnostic tool but a resource to help you better understand your genetic tendencies. Combined with advice from a healthcare professional and other diagnostic methods, it can guide more informed lifestyle and dietary choices. Xcode Life doesn't ship out DNA kits.
Poor health implies that you are physically unwell and experiencing symptoms associated with diseases.
On the other hand, poor wellness means you don't experience any diagnosable symptoms, yet you don't feel content.
This can be due to a poor diet, stress, lack of sleep, and not feeling supported and cared for.
Over time, poor wellness can eventually lead to poor health.
Health is more focused on physical and mental wellness.
It also indicates an absence of signs and symptoms of diseases.
Well-being is not just about being physically or mentally healthy but also experiencing a general satisfaction in life.
You can not be your best healthy self yet feel completely content and safe in life.
Health is a measurable metric, and well-being is a perception.
Although health and wellness are distinct from each other, both of them go hand in hand.
A foundation of good health is essential to achieve wellness, while wellness helps you become healthier.
For instance, not suffering from any digestive issues is health.
However, to maintain this, you must eat a balanced meal full of whole foods, fiber, fresh fruits, and vegetables, which is wellness.
Health care is all about getting treated for your symptoms.
It encompasses diagnosis, medication, surgery, and rehabilitation for a disease.
Wellness care implies focusing on healthy eating, exercise, and stress management.
The health triangle represents a balance between the three aspects of health:
Health and wellness are often used interchangeably.
But they have two distinct meanings.
While health is more about whether you are free from symptoms of certain diseases, wellness incorporates certain practices that keep you healthy.
Health is mainly concerned with the optimum state of your body and mind.
Wellness involves your career goals, social health, relationships, and overall attitude toward life.
Being mindful about your wellness can, in turn, help improve your health.

The 12 Dimensions Of Wellness

7 Best Biohacks For 2025 To Transform Your Health

How Genes and Hormones Interact to Influence Your Health