What Is Anemia?
Anemia is a medical condition characterized by a lack of healthy red blood cells in the body. It is due to low levels of hemoglobin in red blood cells.
Hemoglobin is a protein that carries oxygen and delivers it throughout your body. If it is low, the cells do not get enough oxygen which results in dysfunctional red blood cells.
In the United States, anemia is the most prevalent blood disorder.
Almost 6% of people are affected by this condition.
More than 400 different kinds of anemia exist, and they fall into three categories:
- Anemia due to loss of blood - occurs when there are gastrointestinal conditions, heavy menstruation for women, post-trauma, and use of NSAIDs.
- Anemia due to dysfunctional red blood cells - causes iron-deficiency anemia, sickle cell anemia, megaloblastic anemia, and pernicious anemia.
- Anemia due to the destruction of red blood cells - causes hemolytic anemia when red blood cells burst due to stress.
Causes and Symptoms Of Anemia
Common causes of anemia include:
- Iron deficiency
- Iron is one of the constituents to make hemoglobin. Without enough iron, your body cannot synthesize hemoglobin for red blood cells.
This lack of red blood cells leads to anemia.
- Heavy blood loss from menstrual bleeding, stomach ulcers, and colon cancer depletes the iron content in your body.
- Vitamin (B12 or folate) deficiency
- Next to iron, your body requires vitamin B12 and folate to produce healthy red blood cells.
Lack of this vitamin results in a decreased red blood cell population, further developing anemia.
- People unable to absorb this vitamin from their diet also develop anemia.
- Chronic disorders
- Some chronic conditions, including cancer, HIV/AIDS, rheumatoid arthritis, renal impairment, Crohn's disease, and other acute or chronic inflammatory conditions, could disrupt the synthesis of red blood cells.
- Certain medications
- Non-steroidal anti-inflammatory drugs (NSAIDs) like aspirin or ibuprofen cause ulcers and gastritis.
- Proton pump inhibitors (PPIs) and histamine-2 receptor antagonists are some medications that interfere with digestion or iron absorption.
- These medications cause heavy blood loss resulting in anemia.
- Genetics
- Certain types of anemia are hereditary. Hereditary nonspherocytic hemolytic anemias are hereditary anemias caused by a particular gene mutation.
- Different types of genes cause different types of hereditary anemias.
- The genes that cause mutation are specific to specific hereditary anemia.
You might not even be aware that you have anemia because the symptoms can be so subtle.
As your blood cells disappear, symptoms typically begin to show up.
The following symptoms may occur depending on the cause of the anemia:
- Feeling lightheaded, faint, or loss of consciousness
- Unusual or rapid heartbeat
- Headache
- Pain in your bones, chest, belly, and joints
- Complications with growth in kids and teenagers
- Breathing difficulties
- Cold hands and feet
- Weakness or fatigue
Is Anemia Genetic?
Some forms of anemia can run in families.
The inheritance pattern of anemia can be of two types:
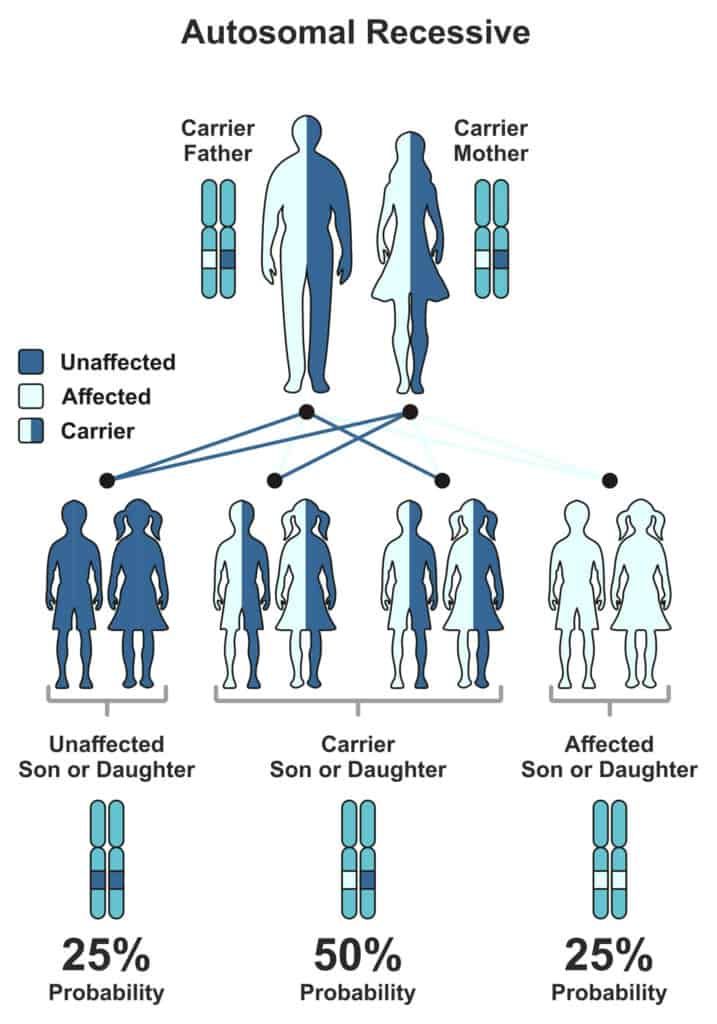
- Autosomal recessive (two copies of a mutation in genes are inherited)
- Autosomal dominant (one copy of a mutation in a gene is inherited)
Types of Anemia That Can Be Inherited
The following types of anemias can be inherited:
Sickle-cell Anemia:
Mutations in the HBB gene cause the blood protein hemoglobin to develop improperly.
Red blood cells become fragile and shrink into a sickle shape, resulting in sickle-cell anemia.
A diminished ability to fight infection and swelling in the hands and feet are further symptoms of sickle-cell anemia.
Sickle cell anemia is inherited in an autosomal recessive manner.
Congenital Pernicious Anemia:
A person with this uncommon kind of anemia is born without the ability to make a protein that aids in the body's absorption of vitamin B12.
You become anemic if your body cannot produce healthy red blood cells due to a lack of vitamin B12.
The Q5R mutation of the intrinsic factor gene causes congenital pernicious anemia.
Additional problems like nerve damage, cognitive issues, and an enlarged liver can result from vitamin B12 deficiency.
Fanconi Anemia:
This particular form of anemia stops the bone marrow from generating new blood cells for the body.
Mutations in FANCA, FANCC, and FANCG genes cause Fanconi Anemia.
People with Fanconi anemia are more susceptible to infection because their bodies do not synthesize enough white blood cells to fight germs.
Hereditary Spherocytosis:
Spherocytes are defective red blood cells inherited from parent to child, which are thin and brittle in this condition.
Hereditary Spherocytosis occurs when red blood cells are destroyed. The majority of hereditary spherocytosis patients only have mild anemia.
Thrombotic Thrombocytopenic Purpura(TTP)
TTP is caused by a certain dysfunctional blood-clotting enzyme, which causes platelets, which aid in wound healing, to cluster together.
People with TTP may endure prolonged bleeding internally, externally, or beneath the skin because their platelets tend to clump together.
It can disrupt red blood cells after leaving the bone marrow and cause breakages in the blood, leading to anemia.
Any condition resulting in the bursting (destruction) of RBCs is known as hemolytic anemia.
Is Iron Deficiency Anemia Genetic?
Iron deficiency anemia can be genetic, as alterations in a person’s genetic code can pass to their child.
Iron-refractory iron deficiency anemia (IRIDA) is due to an inadequate level (deficiency) of iron in the bloodstream. This form of iron deficiency anemia does not respond to iron supplements, as the name suggests.
It is resistant (refractory) to oral iron supplements and only partially responsive to iron supplied in other ways, such as intravenously.
Red blood cells that are excessively tiny (microcytic) and pale (hypochromic) are found with this type of anemia.
TMPRSS6 Gene and Anemia
Mutations in the TMPRSS6 gene cause IRIDA. This gene is in charge of instructing the body to produce the matriptase-2 protein.
Matriptase-2 regulates the body's iron levels.
The body's iron levels can change due to factors affecting this protein.
IRIDA has an autosomal recessive inheritance pattern in which both parents must possess the recessive trait, and the kid must inherit both copies.
The recessive characteristic is only present in one copy of each parent; thus, neither may exhibit any symptoms.
Other Risk Factors for Anemia
A diet deficient in some minerals and vitamins
Your risk of anemia rises if you consume a diet persistently deficient in iron, vitamin B-12, folate, and copper.
Gastrointestinal problems
The risk of developing anemia is high if you have an intestinal condition like Crohn's disease or celiac disease that interferes with the absorption of nutrients in your small intestine.
Menstruation
Red blood cells are lost during menstruation. Therefore, the risk of iron deficiency anemia is generally higher in premenopausal women than in postmenopausal women and men.
Pregnancy
Your risk of anemia increases if you are pregnant without taking a multivitamin with folic acid and iron.
Family History
You may also be more susceptible to the disorder if your family has a history of inherited anemia, such as sickle cell anemia.
Other factors
Your risk of anemia increases if you have a history of certain infections, blood conditions, or autoimmune diseases.
Anemia can result from factors such as alcoholism, hazardous chemical exposure, and pharmaceutical use that decrease red blood cell production.
Age
Anemia risk increases for people over 65.
Summary: Is Anemia Genetic?
Anemia is a blood disorder characterized by dysfunctional or lack of red blood cells.
Common causes of anemia include iron deficiency, vitamin deficiency, chronic disorders, certain medications, and genetics.
Anemia can be inherited in two patterns: autosomal recessive and autosomal dominant.
Some types of anemia that can be inherited include sickle cell anemia, congenital pernicious anemia, Fanconi anemia, hereditary spherocytosis, and thrombotic thrombocytopenic purpura.
Other risk factors of anemia include a poor diet, intestinal problems, pregnancy, age, heavy menstruation in women, family history, etc.