Depression is a serious mental condition that impacts how you feel and the way you think and act.
When left untreated, it can become very disabling, impairing all aspects of human function.
Observational data suggest associations between lower serum vitamin D levels and a higher risk of late-life depression.
Further, lower vitamin D levels may influence the etiology of seasonal affective disorder (SAD).
Some research studies report that people with depression have lower vitamin D levels than those without depression.
But so far, no large-scale study has proven that supplementation with vitamin D or any other vitamin can cure depression.
How Is Vitamin D Produced In The Body?
During exposure to sunlight, the UV-B rays convert a chemical called 7-dehydrocholesterol in the skin into previtamin D3.
Previtamin D3 then travels to the liver and picks up oxygen and hydrogen molecules to become 23-hydroxyvitamin D or 25(OH)D, the active form.
Even though it’s active, 25(OH)D cannot function till it reaches the kidney to acquire the final pair of oxygen and hydrogen.
This forms 1,25 dihydroxyvitamin D/1,23(OH)2D or calcitriol.
How It Works
Calcium is an integral part of our skeletal system and crucial for bone health.
Vitamin D helps the body absorb calcium.
Without this vitamin, only 10-15% of dietary calcium is absorbed (compared to 30-40% with sufficient vitamin D levels).
Low vitamin D levels can increase the risk of fractures, osteoporosis, and other bone conditions.
Recent studies have observed vitamin D receptors (proteins that bind to vitamin D) in several tissues in the body.
The vitamin D receptors are almost omnipresent from the prostate and heart to blood vessels, muscles, and glands.
Research is still underway to find all the roles of vitamin D in the body.
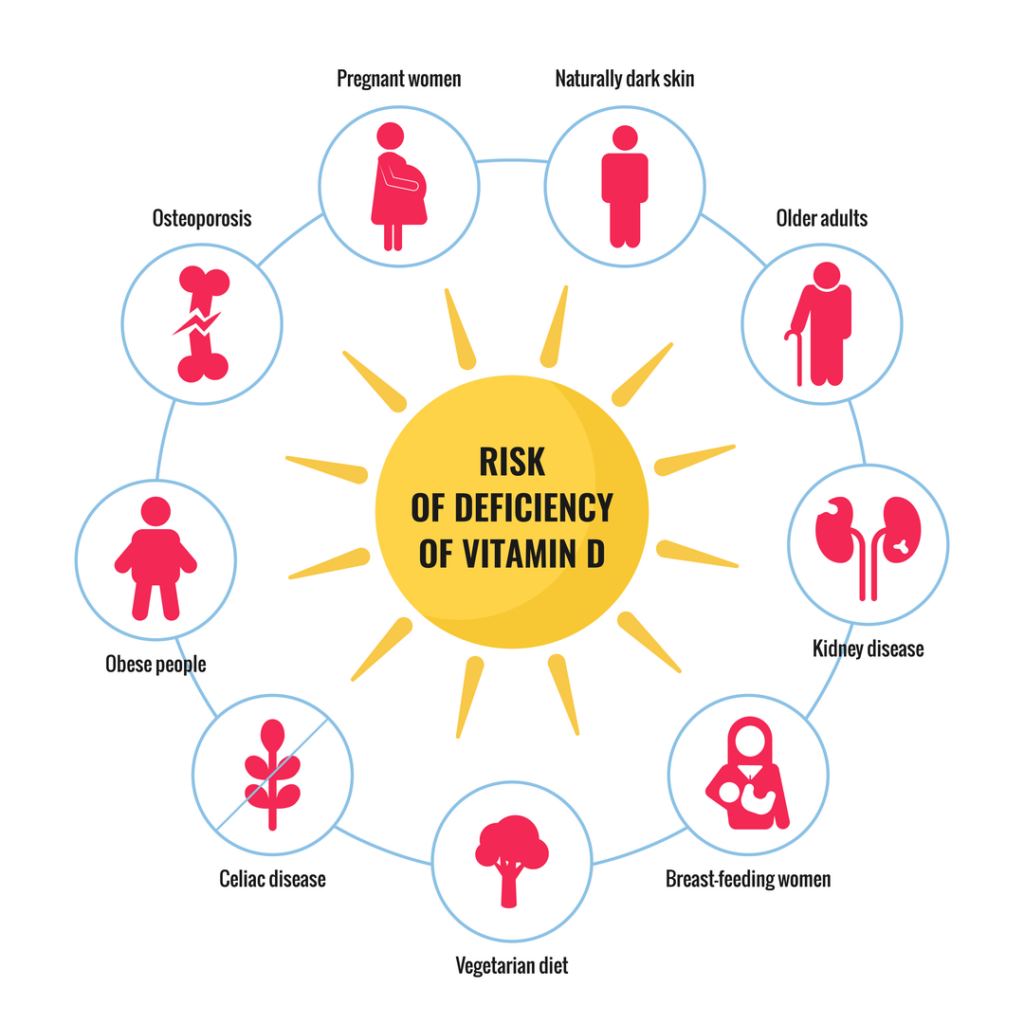
Risk Factors for Vitamin D Deficiency
| Race | Non-Hispanic African-Americans are at the greatest risk for vitamin D deficiency. According to a study, they composed a significant 39.3% of the vitamin D deficient population, compared to only 16.5% of the vitamin D sufficient population. |
| Geography | A study suggests that populations living in any geographic location higher than 35° N are at risk for vitamin D deficiency. Places like North Canada and Alaska, for example, have less access to the UV-B rays. |
| Age | The ability to convert inactive to active vitamin D decreases with age, putting older people at a higher risk for vitamin D deficiency. |
| Skin | Those with darker skin color have more melanin pigments blocking the entry of UV-B rays. Thus, they may be prone to vitamin D deficiency. |
| Pollution | Dust particles can block UV-B rays from reaching the skin. Therefore, those who live in highly polluted may be vitamin D deficient. The deficiency may also be because of the lower inclination to step out in the sun due to higher pollution. |
| Pregnancy & breastfeeding | The demand for vitamin D increases during pregnancy. Following the same diet can result in vitamin D deficiency. Thus, doctors tend to prescribe prenatal supplements with vitamin D in them. |
| Obesity | Fat may interfere with vitamin D absorption. Furthermore, obese people may have mobility issues due to low sun exposure. Those who opt for bariatric surgeries may be at increased risk for malabsorption and subsequent vitamin D deficiency. Those who are overweight but not obese tend to have a lower risk. |
| Absorption issues | Many health conditions like Crohn’s and Celiac disease interfere with nutrient absorption, increasing one’s risk for vitamin D deficiency. |
| Kidney and liver health | The liver and kidneys are two sites in the body where vitamin D is converted into an active and usable form. Any health conditions affecting these organs can increase vitamin D deficiency risk. |
| Smoking | Recent studies have suggested that smoking can reduce vitamin D levels by affecting the ability of sinus mucosa (fluid lining the nasal cavity) to circulate this vitamin. The risk was reduced in former smokers compared to current smokers. |
| Diet | Those who adopt vegetarian and vegan diets without adequate supplementation are at increased risk for vitamin D deficiency. |
| Lifestyle | Any activity that gives less to no room for sunlight can significantly increase vitamin D deficiency risk. Those who wear clothes that cover their whole body for protection or religious reasons get minimal UV-B entry and are prone to deficiency. |
Image: Risk factors for Vitamin D Deficiency
Are Your Genes Preventing You From Getting Enough Vitamin D?
How Much Vitamin D Should I Take? The VDR Gene & Vitamin D Requirements
Vitamin D Deficiency and Depression
Numerous studies have reported an association between vitamin D deficiency and depression.
In particular, prenatal vitamin D deficiency has been connected with postpartum depression.
However, whether it is a causation or correlation relationship remains unclear.
What Does The Research Say?
A few small studies seemed to have observed improvements in depression symptoms upon vitamin D supplementation.
A review of 14 studies involving 31,424 adults by the National Institutes of Health (NIH) reported low vitamin D levels among those with depression.
However, the clinical trials couldn’t back up such findings.
In August 2020, a large study that observed the link between long-term vitamin D supplementation and depression was published in the Journal of the American Medical Association (JAMA).
The trial included 18,353 participants 50 years and older.
None of them had depression or its symptoms at the beginning of the study.
The trial concluded no statistical difference in “the incidence and recurrence of depression or clinically relevant depressive symptoms” throughout the study in the participants who took vitamin D compared to those who took a placebo.
All these results suggest that the link between vitamin D and depression is a correlative relationship.
Those with depression may have low vitamin D levels, but it doesn’t mean the deficiency causes depression.
Possible Explanations
Lesser outdoor time
Severe forms of depression can make it very difficult to get out of bed.
Others may go to work but not participate in any outdoor activities.
Such social withdrawal results in lesser outdoor time and consequently lesser exposure to sunlight.
This can result in vitamin D deficiency.
Poor Diet
Some people with depression may lose appetite, putting them at risk of not eating a balanced diet.
They may also not show much interest in looking for vitamin D-fortified foods.
This may increase the risk for vitamin D and other nutritional deficiencies.
Can Vitamin D Supplements Help Treat Depression?
Even though the jury is still out regarding vitamin D’s effect on depression, research has shown that it is involved in mood regulation.
This could’ve been derived from the observation that our brains have a widespread distribution of vitamin D.
While you can’t tell for sure that vitamin D supplements can treat or help avoid depression, they may help alleviate the symptoms.
It is important to consult a doctor and get a blood test (if required) before getting started on a vitamin D supplement.
Both vitamin D2 and D3 work well as supplements.
D2 is derived from plants, while animal sources produce D3.
It is important to understand that amping up your vitamin D is not a replacement for seeing a mental health care provider to help treat depression.
Summary
We obtain most of the vitamin D via UV-B rays from the sun. Certain food items provide vitamin D as well. Certain groups of the population (dark-skinned, older, living in the northern regions, obese) may be at higher risk for vitamin D deficiency. Though a few small studies have linked vitamin D with depression, there’s still no clarity on whether there’s a causal relationship between the two. Vitamin D may not treat or prevent depression, but studies reveal that supplementation and sun exposure are effective ways to help regulate the mood.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2908269/
- https://jamanetwork.com/journals/jama/fullarticle/2768978
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6075634/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4772204/
- https://pubmed.ncbi.nlm.nih.gov/24698317/
- https://pubmed.ncbi.nlm.nih.gov/29958055/
- https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/
- https://jamanetwork.com/journals/jama/fullarticle/2768978
- Vitamin D Deficiency Due To Genetics: The VDR and GC Genes