Blood clotting is an important process that keeps you from losing a lot of blood when you have an injury. But what if they happen too often and last too long? Thrombophilia, a condition characterized by frequent blood clot formation, can be life-threatening if left untreated. Fortunately, both acquired and hereditary thrombophilia can be managed with blood thinners in most cases. This article will explore the genes and changes in them that may increase your risk for this condition.
Did You Know? Your ancestry test DNA data includes 700,000 markers, which can be used to learn everything from disease risk and drug sensitivities to nutritional requirements and fitness parameters. Learn more. Here's how 23andMe and AncestryDNA users have benefited from uploading their DNA data to Xcode Life
What Is Thrombophilia?
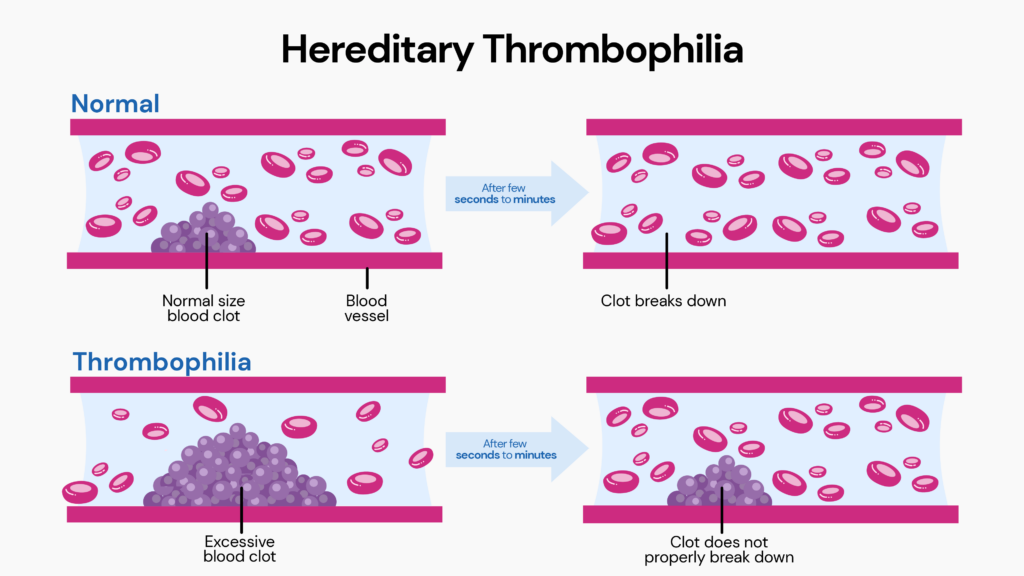
Thrombophilia is a blood clotting disorder that increases the risk of blood in veins and arteries clotting.
This condition is also called ‘hypercoagulable’ as it causes the blood to clot more easily.
When blood clots occur due to thrombophilia, they block the arteries and veins, preventing adequate blood supply to or from organs and tissues.
Causes
One of the main causes of thrombophilia is genetics. However, it may be caused by other factors too.
A few medical conditions that may cause thrombophilia include:
- Antiphospholipid syndrome (APS)
- Hepatitis
- Liver diseases
- HIV
- Disseminated intravascular coagulation (DIC)- a rare clotting disorder
Symptoms And Characteristics
Thrombophilia does not cause signs or symptoms until it forms a clot that affects an organ or tissue.
The signs and symptoms depend upon the organ or tissue affected by the blood clot.
Deep vein thrombosis
One of the most common presentations of thrombophilia is the development of a clot in a vein, causing Deep Vein Thrombosis (DVT).
DVT can occur anywhere in the body but most commonly affects the large veins in the leg.
A few symptoms that may occur due to DVT are pain and swelling in the leg.
Pulmonary embolism
If the blood clot travels to the lung, it can result in pulmonary embolism.
Symptoms you may experience due to this condition include chest pain, breathing difficulty, shortness of breath, painful deep breathing, and an increased heart rate.
Blood clot in the abdomen
Nausea, vomiting, and pain in the region are the most common symptoms of thrombophilia.
Blood clots in the heart
If a blood clot develops or travels to the heart, you may experience chest pain, shortness of breath, sweating, nausea, and lightheadedness.
Types Of Thrombophilia
Thrombophilia can be acquired or genetic (inherited).
Acquired Thrombophilia
This type of thrombophilia is more common than the inherited type.
It is said to be ‘acquired’ as one acquires it during their lifetime due to lifestyle factors, medications, or other diseases.
The most common type of acquired thrombophilia is antiphospholipid syndrome.
Hereditary Thrombophilia
As the name suggests, this form of thrombophilia occurs due to the inheritance of affected genes from one or both parents.
People who inherit the affected genes are unable to make one or more clotting factors, which results in thrombophilia.
For example, some women who have had recurrent miscarriages before the age of 40 years may have inherited thrombophilia.
There are different types of hereditary or genetic thrombophilia:
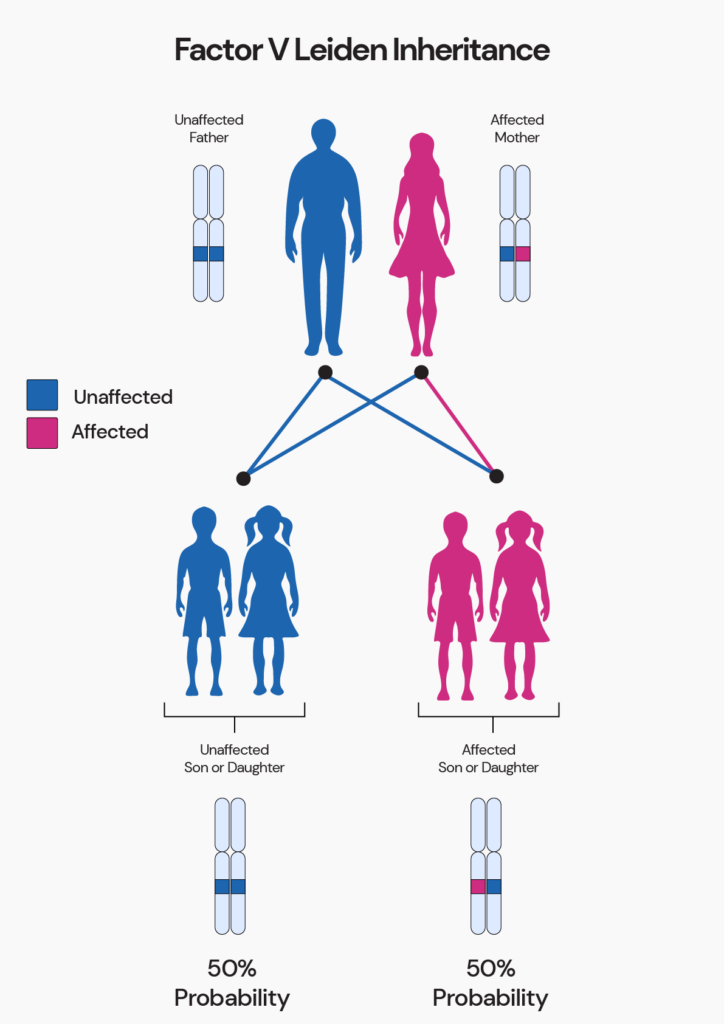
- Factor V Leiden Thrombophilia
This is the most common form of genetic thrombophilia, affecting 1% to 5% of the population.
Factor V Leiden is the name given to a specific gene mutation that results in thrombophilia.
People with this type of genetic thrombophilia have a higher risk of getting first-event DVT but not repeated blood clots thereafter. - Prothrombin Thrombophilia
A relatively common type, prothrombin thrombophilia affects 1% to 5% of the general population.
People with this condition are at high risk for first-event pulmonary embolism, deep vein thrombosis, and miscarriage but not repeated blood clots thereafter. - Protein C deficiency
This type of genetic thrombophilia affects less than 1% of people and puts them at high risk for repeated blood clots.
Protein C deficiency is not as common and affects less than 1% of people.
This type of thrombophilia increases your risk of repeated blood clots. - Protein S Deficiency
A rare form of genetic thrombophilia, protein S deficiency affects less than 1% of people.
When inherited from both parents, the affected (or mutated) gene may cause a life-threatening blood clotting issue in infants. - Antithrombin deficiency
This form of thrombophilia affects 1 in 500 to 5,000 people.
Over 80% of people with this form of thrombophilia get at least one clot by the age of 50.
Genetics Of Hereditary Thrombophilia
Hereditary thrombophilia is genetic.
Two of the most common genetic variants associated with hereditary thrombophilia are found in two genes - F5 and F2.
Both these genes are required for the normal clotting process.
F5 Gene
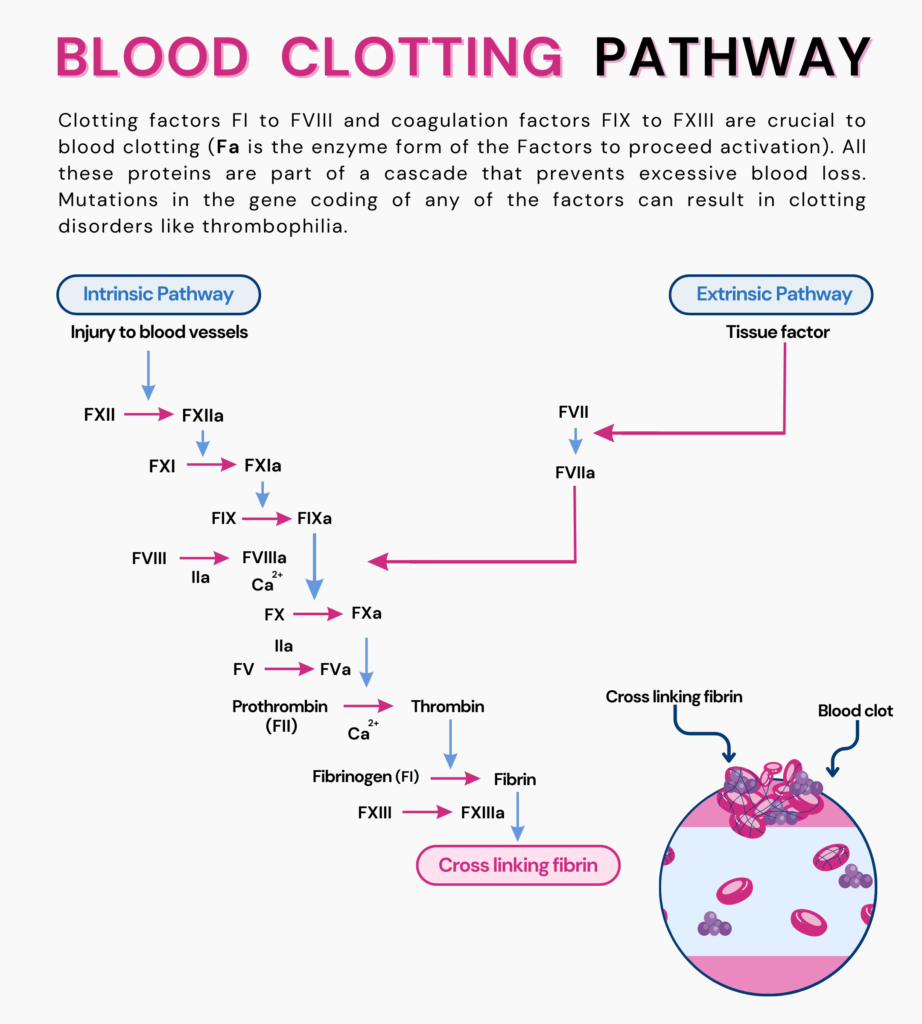
The coagulation or blood clotting system in the body is controlled by several proteins and molecules.
The F5 gene provides instructions for making a protein called coagulation factor V.
This protein circulates in the blood in its inactive form till it reaches the liver, where it is activated.
When activated coagulation factor V combines with activated factor X, they form a complex that converts prothrombin to its active form, thrombin.
Thrombin, in turn, converts a protein fibrinogen to fibrin, which is what forms a blood clot.
Coagulation factor V also has another role.
It regulates the clotting mechanism by interacting with activated protein C (APC).
This protein inactivates coagulation factor V, slowing the clotting process and preventing clots from growing too large.
However, in some people with factor V Leiden thrombophilia, coagulation factor V cannot be inactivated by APC.
Due to this, the process of clotting remains active for longer, increasing the risk of developing abnormal clots.
F2 Gene
The F2 gene is responsible for coagulation and maintenance of vascular integrity.
It also provides instructions for making the protein prothrombin (or coagulation factor II).
Prothrombin thrombophilia is caused by an abnormal change (or mutation) in one of the building blocks of the DNA in the F2 gene.
This causes the F2 gene to be overactive and produce more prothrombin.
An abundance of prothrombin means excess thrombin, fibrinogen, and fibrin (or clot).
So, the presence of the F5 variant (or the factor V Leiden) and the F2 variant of the genes increase the risk of blood clot formation that can block blood flow to different parts of the body.
In some cases, thrombophilia may be due to large deletions or duplications in the following genes:
- F5
- SERPINC1
- PROS1
- PROC
- F9
- FGA
- FGB
How’s It Inherited?
Thrombophilia may have an autosomal dominant, autosomal recessive, or X-linked inheritance.
Is Thrombophilia An Autoimmune Disease?
Antiphospholipid syndrome (APS), the most common and aggressive form of acquired thrombophilia, is an autoimmune disease.
It is a condition that causes blood clots to form in the blood vessels and causes serious health problems.
In APS, the body’s immune system attacks a type of fat molecule called phospholipids.
Phospholipids are found on the surface of many cells, including those lining the blood vessels.
This causes abnormal blood clots to form in the blood vessels.
Other Risk Factors Of Thrombophilia
Besides genetics, a few factors that may increase one’s risk of developing thrombophilia are:
- Pregnancy
- Overweight or obesity
- Sedentary lifestyle
- Using tobacco products
- Birth control pills that contain estrogen
- Other health conditions like atherosclerosis, diabetes, cancer, or heart problems
- Hormone replacement therapy (HRT)
Complications Of Thrombophilia
Since blood clots can affect any blood vessel in the body, they can prevent the smooth flow of blood to many tissues and organs.
This can lead to complications like:
- Pulmonary embolism of the lungs
- Heart attack
- Stroke
- Kidney failure
- Deep vein thrombosis (DVT)
- Miscarriage
- Peripheral artery disease (PAD)
Diagnosis, Management, and Treatment of Thrombophilia
Diagnosis
A thorough medical history, a physical examination, and blood tests to check for a genetic cause of thrombophilia can help diagnose thrombophilia.
Your doctor may recommend genetic testing if someone in your family has thrombophilia.
Besides blood and genetic testing, your doctor may also advise angiograms, venograms, or an ultrasound to detect the presence of clots in your blood vessels.
Treatment and management of thrombophilia
There is no cure for genetic or hereditary thrombophilia.
However, the signs and symptoms can be effectively managed with:
Medications
Medications routinely used for treating thrombophilia include anticoagulants like heparin and warfarin.
Warfarin is an oral drug that takes a few days to show its effects.
When you have many clots that need urgent treatment, you may need a fast-acting drug like heparin that is usually injected.
Use of compression stockings
Both types of thrombophilia may require the use of compression stockings for your legs to prevent the breaking up of a clot.
Some people may require surgery to remove the clot.
Practice healthy lifestyle habits
If you have thrombophilia, you must make a few lifestyle changes, like eating a nutritious diet, maintaining a healthy weight, exercising regularly, and avoiding long periods of rest or inactivity.
These tests usually include a prothrombin time test and an international normalized ratio (INR).
What Foods Should You Avoid If You Have Thrombophilia?
If you have thrombophilia, your doctor will advise you to eat a healthy diet.
Here are some foods that you may need to stay clear of:
- Refined and processed foods
- Food high in sugars, including sugary beverages
- Red and processed meats
- Go easy on the salt
- Avoid alcohol consumption (as it may interfere with the blood thinner medication)
If you are on blood thinners like warfarin, you must consume foods rich in vitamin K in moderation.
This is because vitamin K is known to interact with warfarin.
Summary
- Clotting is the body’s natural mechanism, but some people lack certain blood molecules that help to clot.
- Thrombophilia is a blood clotting disorder that increases the risk of blood in veins and arteries clotting.
- Thrombophilia can be genetic when inherited from one or both parents or can develop due to other health conditions.
- Genetic thrombophilia can be of different types, with factor V Leiden being the most common.
- Genetic mutations in the F5 and F2 genes are the two most common variants associated with genetic thrombophilia.
- Not treating thrombophilia in time can result in complications like deep vein thrombosis, pulmonary embolism, stroke, heart attack, and kidney failure.
References
- https://my.clevelandclinic.org/health/diseases/21797-thrombophilia
- https://medlineplus.gov/genetics/condition/factor-v-leiden-thrombophilia/
- https://emedicine.medscape.com/article/211039-overview
- https://www.uptodate.com/contents/inherited-thrombophilias-in-pregnancy
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1592479/
- https://www.ahajournals.org/doi/10.1161/JAHA.119.012877
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7233636/




