Corneal thickness is an important factor in diagnosing and managing glaucoma. Measuring the thickness of the cornea can help to identify early signs of the disease and determine the best course of treatment. A thin cornea is more susceptible to damage from high intraocular pressure, a common glaucoma symptom. This makes early detection and treatment of the disease essential to preserving vision.
The Gene Health Report Covers Glaucoma and 50 Other Health Conditions
Xcode Life's Genetic Glaucoma DNA Report
Researchers have identified a number of genes associated with glaucoma.
In the sample report below, we've attempted to analyze some important genes that increase the risk of glaucoma.
You can identify your genetic risk of glaucoma by using your 23andMe DNA data and placing an order for the Gene Health Report.

What Is Corneal Thickness?
Corneal thickness is a measure of the distance from the front surface of the cornea to the back surface of the cornea.
The average thickness of a human cornea is about 0.5 mm.
It is important because it affects how light travels through the eye and how well the eye can focus.
Corneal Thickness and Intraocular Pressure
Corneal thickness can affect eye pressure reading.
Also called intraocular pressure (IOP), eye pressure is a measure of fluid pressure inside the eye.
Accurate and precise IOP readings are crucial to evaluate a patient's risk of progressive optic nerve damage.
It is an important reading taken during ophthalmic evaluations, especially for people with ocular hypertension and glaucoma and people at risk for glaucoma.
When the cornea is thinner than normal, it can result in an underestimation of the IOP, and when it’s thicker, it can result in an overestimation.
This can affect the diagnosis and treatment of glaucoma and ocular hypertension.
Corneal Thickness and Glaucoma: What’s The Link?
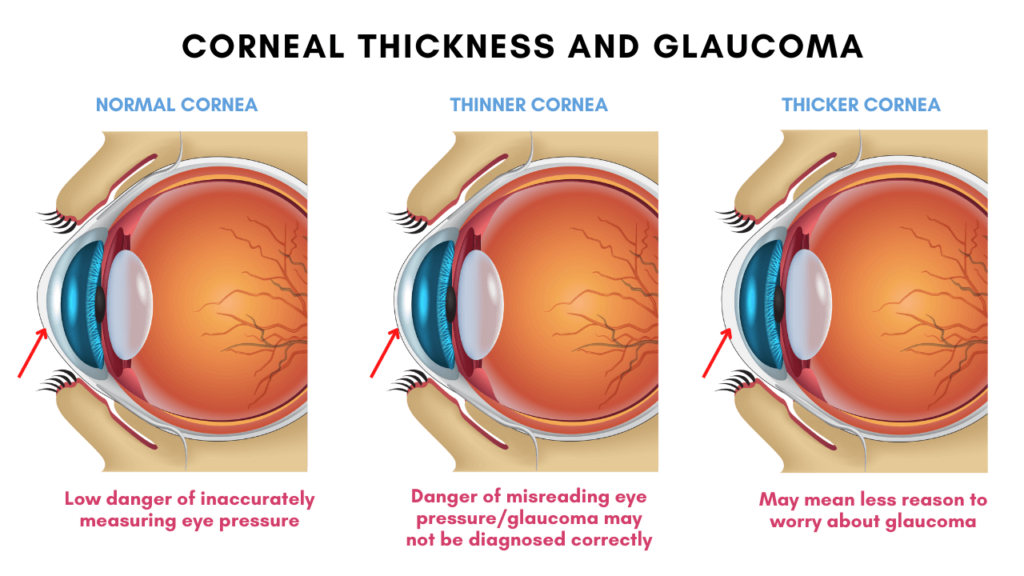
Corneal thickness has been hypothesized to be a risk factor for glaucoma.
A thinner cornea increases the risk of developing glaucoma and its rapid progression.
However, whether the corneal thickness is a true independent risk factor for glaucoma remains unanswered.
A study published in the Ophthalmology journal attempted to address this.
According to the results, corneal thickness as a prognostic factor of glaucoma doesn’t entirely revolve around its effect on the IOP measure.
Rather, it influences other structural and physical factors that affect the pathogenesis of glaucoma.
The Genetics Behind It
Central corneal thickness (CCT) is one of the most heritable human traits with a strong genetic component.
Despite its high heritability, until recently, studies could explain only 8.5% of the variance in CCT.
This includes 44 genomic loci (or locations in a gene).
A large study involving nearly 45,000 individuals attempted to identify additional genetic links to CCT.
The researchers discovered 98 genomic loci, 41 of which haven’t been identified in previous studies.
This study helped explain 14.2% of the variance in CCT.
Among these loci, a variant in the RAPSN gene (indicated as rs3740685) was significantly associated with glaucoma.
Summary
Corneal thickness affects how light travels through the eye.
It can lead to incorrect intraocular pressure readings (IOP), an important measurement criterion for glaucoma.
A thinner cornea has been associated with an increased risk for glaucoma.
However, studies suggest that corneal thickness affects the prognosis of glaucoma not only through IOP but also through other physical and structural changes associated with glaucoma.
Corneal thickness has a significant heritable component, and studies have been able to explain a 14.2% variance.




