Estimated reading time: 6 minutes
Key Takeaways
- Research confirms that insomnia is genetic in nature, with heritability accounting for 31–58% of an individual's risk.
- Having a parent or sibling with insomnia significantly raises your own likelihood of developing the condition.
- The MEIS1 gene is among the strongest genetic contributors, with specific variants linked to a higher risk of insomnia symptoms.
- Beyond genetics, factors like age, sex, and conditions such as anxiety or heart disease can further elevate insomnia risk.
What is Insomnia?
Insomnia (also known as sleeplessness) is a common sleep disorder that is characterized by the inability to fall asleep or stay asleep at night, resulting in tired or unrefreshing sleep.
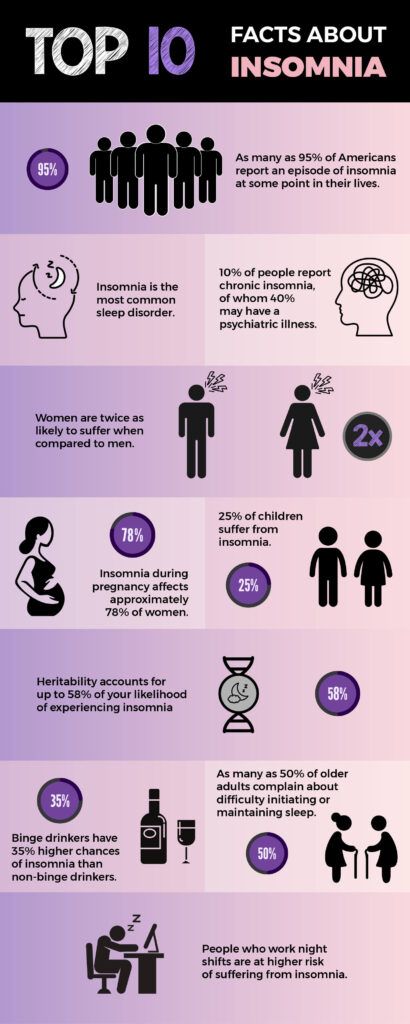
According to the American Psychiatric Association (APA), insomnia is the most common sleeping disorder.
Research indicates that approximately 10% of adults worldwide meet the criteria for chronic insomnia.
Approximately 30% to 40% of adults in the United States report occasional symptoms of insomnia.
A diagnosis of insomnia needs to meet the following two categories:
- Difficulties in sleep for at least three nights a week for a minimum of three months
- Difficulties in sleep that result in functional distress in the individual’s life
This can be caused by variations in biological, psychological, and social factors, which most often result in a reduced amount of sleep.
Is Insomnia Genetic?
People with parents or siblings with insomnia have an increased risk of experiencing the condition themselves. This indicates a genetic link to insomnia.
This was further confirmed by a 2018 study that reported that insomnia has a partially heritable basis. In fact, heritability accounts for 31% to 58% of your insomnia risk.
Insomnia also appears to share genetic links with other health conditions.
The researchers also found a strong genetic link between insomnia and type 2 diabetes.
Tissue-specific gene-set analyses showed that insomnia might have higher genetic signals among genes that are usually expressed in the brain.
The functions of these regions of the brain are of relevance to insomnia.
The genetic correlations between insomnia and psychiatric traits were stronger than the genetic correlations between insomnia and other sleep-based characteristics.
The study suggests that, genetically, insomnia resembles neuropsychiatric traits more closely than other sleep-related characteristics.
MEIS1 Gene and Insomnia
The MEIS1 gene is a transcription factor that plays a key role in hematopoiesis, endothelial cell development, and vascular patterning.
It also plays a role in neurodevelopment.
Research studies have shown that the reduced MEIS1 levels and function of the gene may contribute to the pathogenesis of sleep-related disorders.
rs113851554 And Insomnia Risk
The rs113851554 is a G>T polymorphism located in the MEIS1 gene, which is found to be correlated with multiple sleep disorders.
A study found that the T allele of rs113851554 is associated with an increased risk of developing insomnia symptoms.
Functional study analysis suggested that the rs113851554 in the MEIS1 locus is most strongly associated with insomnia disorder.
Current Research on 'Is Insomnia Genetic?' - 2026 Updated
A 2026 review published in Frontiers in Medicine evaluated 105 Mendelian randomization studies.
This research indicates that genetic susceptibility to insomnia causally increases the risk of developing over 30 chronic conditions. These conditions include coronary heart disease, severe depression, and type 2 diabetes.
Additionally, integrative genomics research analyzing over 386,000 individuals identified 449 genes associated with insomnia risk. The study prioritized five promising genes: DALRD3, LDHA, HEBP2, TEX264, and FGFR3.
These genes may help explain the underlying biological mechanisms and altered brain functions involved in the disorder.
While these studies confirm a strong genetic link, insomnia genes are non-deterministic.
Individual sleep patterns vary greatly because genetic risk factors interact with environmental and lifestyle variables.
A genetic predisposition suggests susceptibility, but it does not guarantee an individual will develop clinical insomnia.
More Than 50% Of Sleep Issues Are Rooted In Genetics
Upload your existing 23andMe or Ancestry DNA data to uncover sleep risks, nutrition factors affecting rest, and personalized solutions, all in one $199 report pack.
50,000 users globally. Rated 4.6/5
Other Risk Factors for Insomnia
Insomnia is more common in women than in men.
More than one in four women in the United States experience insomnia, compared with fewer than one in five men.
Insomnia is more common in older people than in younger ones.
As many as 50% of older adults complain about difficulty initiating or maintaining sleep.
Medical and psychiatric conditions can increase insomnia risk.
Insomnia is more commonly seen in those with heart disease, asthma, depression, and anxiety than their healthier counterparts.
Effects Of Insomnia On Health
- Increased risk of heart disease, stroke, inflammation, obesity, seizures, diabetes, and asthma
- Increased risk of anxiety and depression
- A negative impact on your memory
- Harder to concentrate and be productive during the day
- More prone to falling and accidents by affecting your balance
- Lowered life expectancy
Tips To Prevent And Manage Insomnia
- Having a consistent bed time can help stabilize your sleep cycle, making it easier to fall asleep.
- Frequency daytime naps can result in difficulties falling asleep at night.
- Experts recommend waiting at least three hours after you've eaten to go to bed.
- Daily physical activity can help with energy expenditure, improving both sleep onset time and sleep quality.
- Stress management through meditation, yoga, and therapy can help calm your mind and prepare it for a restful night of sleep.
- If lifestyle changes don’t fix your insomnia, seeking professional help can help you sleep better.
Yes, insomnia has a strong genetic component. Research indicates heritability accounts for 31–58% of an individual's risk though genes alone do not determine outcomes.
No, your severe lack of sleep is almost certainly common, treatable insomnia rather than the exceptionally rare genetic disease FFI.
No, while DNA tests can highlight natural genetic predispositions to sleep issues, they cannot medically diagnose the definitive root cause of your clinical insomnia.
Yes, a genetic susceptibility to insomnia directly increases your risk for developing conditions like type 2 diabetes, coronary heart disease, and depression.
Yes, you can absolutely overcome it; Cognitive Behavioral Therapy for Insomnia (CBT-I) is a highly effective, gold-standard treatment regardless of your genetic background.
Research suggests diet can influence insomnia symptoms. A 2024 meta-analysis of 591,223 individuals found high-quality diets linked to a 34% lower risk, while unhealthy dietary patterns raised risk by 20%.
CBT-I (Cognitive Behavioral Therapy for Insomnia) is the most evidence-based treatment for insomnia, carrying a strong recommendation in AASM guidelines.
Summary
- Insomnia is the most common sleeping disorder and describes the inability to fall asleep or stay asleep at night.
- Insomnia can be caused by variations in biological, psychological, and social factors, resulting in a reduced amount of sleep.
- Over 300 genes have been identifed in association with insomnia. The MEIS1 gene has one of the strongest associations with insomnia and is known to contribute to the pathogenesis of sleep-related disorders.
- Sticking to a proper routine, exercising, avoiding many day time naps, stress management, and seeking professional help can help treat and manage insomnia.
References
https://pubmed.ncbi.nlm.nih.gov/30804565/
https://pubmed.ncbi.nlm.nih.gov/26132482/
| Expert picks: What To Read Next |
|---|
| What Is The Best Sleeping Position For Lower Back Pain? |
| Why Do I Keep Waking Up At 4 AM? |