Less than 2% of the global population carries the red hair gene, one of the most intriguing human traits. It may seem like common knowledge that red hair originated in the Viking lands of Scandinavia. However, research points to red hair originating in Central Asia as a mechanism against the harsh sun. Eventually, it spread to remote regions like Ireland, Scotland, and Scandinavia, where it is most abundant today. This article will help you learn more about the red hair gene: why some people have red hair, how the gene travels down generations, how red hair can affect your skin, and how to know if you could be a carrier of the gene.
Melanin, a coloring pigment produced by the melanocyte cells in the hair, determines hair color.
When melanocytes produce an excess of eumelanin, a dark-colored melanin pigment, people get black or brown hair.
Those who don’t produce enough of this pigment have blond hair.
In rare cases, the melanocytes produce another pigment called pheomelanin.
Pheomelanin is a yellow/reddish pigment responsible for the iconic red-colored hair.
The type of melanin pigment the melanocyte cells produce depends on a person’s genes.
Image: Types of Melanin Pigments
The MC1R gene is one of the strongest influencers of red hair.
Thus, it is also called the red hair gene.
It instructs your body to produce the melanocortin-1 receptor that decides which type of melanin the melanocytes produce.
When the receptor is active, it encourages the melanocytes to produce eumelanin, leading to darker hair color.
When the receptor is blocked or inactive due to mutations in the MC1R gene, it produces pheomelanin instead, leading to reddish hair color.
Pheomelanin production causes individuals to grow red hair.
Red hair is a recessive genetic trait.
This means that a person must inherit the genetic change associated with red-colored hair from both biological parents for it to be active.
Many people may be carriers of one copy of the mutated gene and still have darker hair color.
A study reports that up to 40% of people in Scotland carry at least one copy of the mutated gene despite only 13% having red hair.
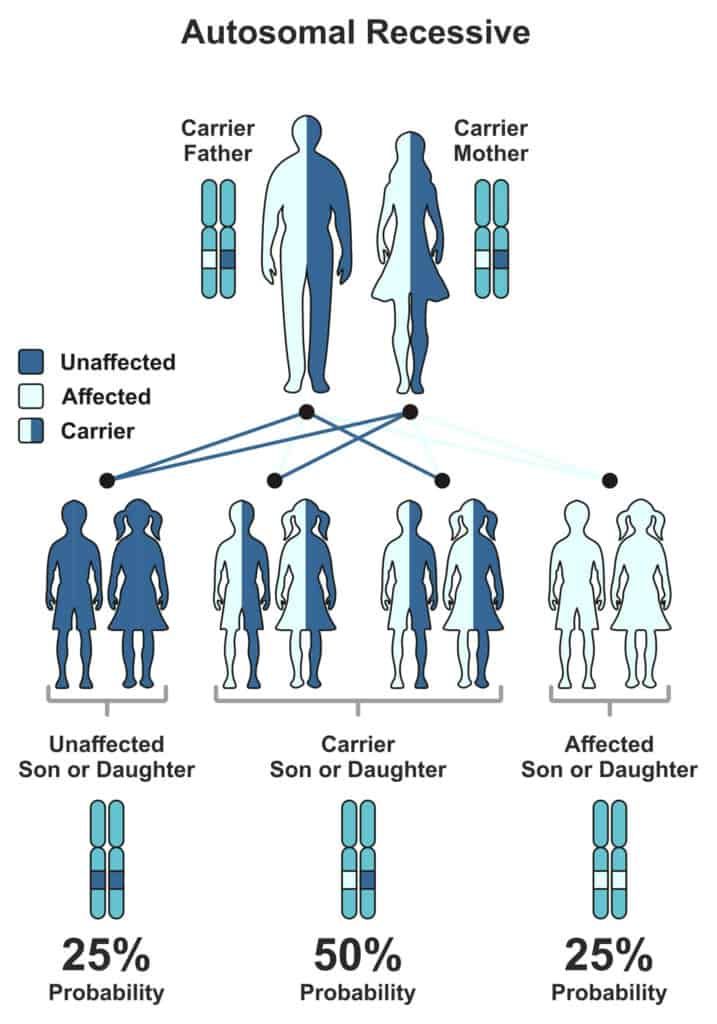
In some families, a child could mysteriously be born with red hair despite generations of people having darker hair.
The darker hair implies that the previous generations were all silent carriers of the gene.
Genetic testing could predict an interesting turn of events like this.
Genetic testing can identify if the parents are carriers of the MC1R gene mutations and predict whether a child will have red hair.
The effects of carrying the MC1R gene don’t end with the hair alone.
A few conditions seen in such individuals include:
Genetic testing to know whether you carry the red hair gene is thus beneficial for you and your future generations.
The following scenarios will help you understand your likelihood of having a child with red hair.
Each scenario has a different genetic makeup of the biological parents involved.
Both parents have dark hair.
In this case, there is a practically 0% chance that your child will be red-haired.
Both parents have dark hair and carry one copy of the gene each.
In this case, there is a 25% chance that the child will have red hair and a 50% chance that the child may have dark hair but carry the red gene.
One parent has two copies of the gene, and the other has none.
In this case, the children may carry the red hair gene but will not have red hair.
In this case, there is a 50% chance the child will be red-haired and another 50% chance that the child will be dark-haired and a carrier of the red hair gene.
In this case, all the children will also have red hair.
Millions of Americans unwittingly endure glaucoma, an invisible cause of vision problems every year. The early symptoms of glaucoma can be hard to diagnose, so people don’t usually find out until it’s too late. Genetic mutations are one of the leading causes of glaucoma, and regular genetic and eye testing can help diagnose it in time, especially for those with a positive family history of the disease. Read on to learn about glaucoma, its genetic risk factors, its causes, and how to identify if you’re at risk.
Glaucoma is a hereditary condition that damages the optic nerve.
This nerve sends visual signals from the eye to the brain, helping you understand what you see.
Glaucoma progresses slowly. There are no clear early signs of this disease, and most people don’t seek medical attention until they notice a decline in their vision.
People with a genetic risk for the condition may need regular eye exams to monitor their optic nerve health and intraocular pressure (IOP).
High IOP is the main culprit of glaucoma.
A lubricant called aqueous humor circulates within the anterior chamber of the eye. In order to maintain a stable IOP, it is drained out of the eye regularly.
If this drainage system is blocked, the aqueous humor builds up in the eye, increasing the IOP.
Pressure builds on the optic nerve, gradually causing the death of optic nerve fibers, leading to blind spots and poor vision.
Research has shown that some forms of glaucoma are hereditary and can be passed down through generations.
Glaucoma is inherited in either an autosomal dominant or autosomal recessive manner.
In autosomal dominant inheritance, only one copy of the mutated gene from either parent is needed to express itself in both the parent and the offspring. Juvenile glaucoma is inherited in this manner.
In autosomal recessive inheritance, both parents must carry one copy of the mutated gene (in its recessive state), and the child must inherit both copies to be at risk for glaucoma. Congenital glaucoma is inherited in this manner.
Some variants of glaucoma may run in the family. The parents may be carriers of the mutated genes and not develop the condition themselves while passing it on to their children.
Sometimes, existing risk factors like hypertension, hypotension, diabetes, age, or eye injury in families could lead to the development of glaucoma.
A meta-analysis studied 46 published observational research papers to find gender-based risk factors for developing OAG.
The results found that men were 1.4 times more likely to develop glaucoma than women.
The myocilin (MYOC) gene produces the myocilin protein, which is essential for maintaining IOP.
Scientists have identified at least a hundred variations of the MYOC gene.
These variations may lead to the underproduction of myocilin, leading to increased intraocular pressure and glaucoma.
About 4% of all cases of primary OAG and more than 10% of all cases of juvenile OAG are due to MYOC mutations.
The Cytochrome P450 family 1 subfamily B member 1 (CYP1B1) gene produces the CYP1B1 enzyme.
Researchers have studied over 100 variations of this gene.
50% of all cases of primary congenital glaucoma are due to mutations in this gene at the GLC3A locus.
The Latent Transforming Growth Factor Beta Binding Protein 2 (LTBP2) gene produces the LTBP2 protein, which forms the anterior chambers of the eye.
A study found that null mutations in this gene could lead to an increased risk of developing PCG.
While these 3 are the most researched genes for glaucoma, other genes also play a minor role in causing the disease.
Changes in certain genes can increase your risk for many chronic health conditions, including glaucoma. Learn more:
Increased IOP slowly damages the optic nerve over time, leading to open-angle glaucoma (OAG)
Though it doesn’t show early symptoms, it could lead to blurry vision and the gradual loss of both peripheral and central vision.
A 2011 study reports that single-gene mutations cause 5% of all POAG.
For instance, mutations in the MYOC gene can cause juvenile open-angle glaucoma.
Multiple mutations and environmental risk factors can lead to the other 95% of cases.
Early-onset glaucoma is a type diagnosed before the age of 40 in adults.
This type is primarily hereditary and may occur even without related risk factors.
A majority of early-onset glaucoma cases turn out to be primary open-angle glaucoma.
Early-onset glaucoma is generally inherited in an autosomal recessive manner- meaning that while parents may carry one copy of the gene, the disease will not be inherited unless the child carries both copies.
Congenital glaucoma occurs in infants before the age of three, leading to optic nerve damage and vision loss.
Infants with congenital glaucoma generally exhibit red or cloudy eyes, an increased rate of blinking, light sensitivity, and tear production without crying.
Congenital glaucoma could be due to complications affecting the infant’s eye as a fetus.
Studies say that variations in the CYP1B1 or LTBP2 genes could lead to the development of primary congenital glaucoma in infants under the age of three.
Juvenile OAG (JOAG), diagnosed in childhood or early adulthood, is called juvenile open-angle glaucoma.
The cause and prognosis of the disease are the same.
Juvenile OAG is inherited in an autosomal dominant manner, meaning that if even one parent carries a MYOC gene with the specific mutation responsible for JOAG, the child will end up with JOAG.
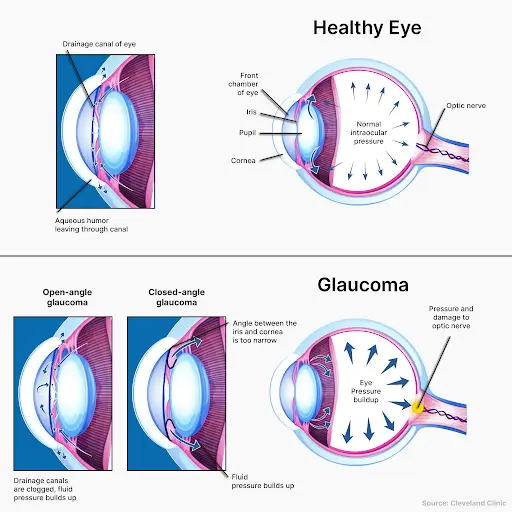
Angle-closure glaucoma (ACG) occurs when the IOP suddenly increases, stopping the movement of the aqueous humor in the eye.
Since this is an acute attack, it presents with headaches, nausea, and eye pain. The vision turns blurry, and halos are visible around light sources.
ACG generally presents in one eye at a time. With timely medical aid, doctors could save the other eye.
Interestingly, normal-tension glaucoma damages the optic nerve without an increase in IOP.
Instead, normal-tension glaucoma could develop due to poor blood flow to the optic nerves or some other inherited trait.
Secondary glaucoma is the development of either open-angle or angle-closure glaucoma due to a separate condition, such as:
Analyzing your genes can also help you understand your risk of developing the disease.
Genetic testing is beneficial in identifying early-onset glaucoma if the condition begins manifesting itself in people under 40 years of age.
Suppose genetic testing reveals a higher risk of developing glaucoma. In that case, you may need regular eye exams done by an eye doctor to diagnose the condition before it worsens.
In fact, a comprehensive eye exam once every two years can be beneficial to anyone whose first-degree relatives are diagnosed with glaucoma.
Water helps lower IOP if consumed in moderation. Drinking too much water in a short time can lead to increased IOP.
Glaucoma is not a fatal condition. It will neither increase your mortality risk nor lead to fatal complications.
Stress does not directly lead to open-angle glaucoma. However, patients who are regularly overwhelmed may neglect their treatment courses, which could worsen their condition.
Tomatoes, a staple in everyone's pantry, and potatoes, a cult favorite, along with eggplants and peppers, belong to the nightshade family of vegetables. However, what's a delicious ingredient for many can be a source of discomfort for some. Experiencing symptoms like redness, itching, or digestive issues after a meal featuring these foods might point to a lesser-known but significant condition: a nightshade allergy. This comprehensive article covers everything you need to know about nightshade allergies, from the underlying causes and risk factors to the intricate genetics and effective management strategies.
Did You Know?
Genetic changes are the most common cause of food and other allergies. Using your existing DNA raw data file, you can find out which food, environmental, and drug allergies you're susceptible to. Learn more.
Nightshades are part of the Solanaceae family, consisting of 3000 flowering plants. Although some of these plants are beneficial, some can be dangerous if consumed.
For instance, belladonna, a deadly nightshade, increases heart rate and blood pressure.
Tobacco is a nightshade plant used to make cigarettes.
Yet, many nightshades, such as tomatoes, eggplants, potatoes, and bell peppers, are staple foods in various cuisines across the globe.
Nightshades are rich in potassium, iron, fiber, vitamin C, and antioxidants such as anthocyanins and lycopene.
They are beneficial for heart health and cancer prevention.
However, some people exhibit adverse effects after eating nightshades.
This condition is called nightshade allergy, intolerance, or sensitivity.
Nightshades possess certain chemical compounds that may be harmful to some people.
These chemicals, called phytochemicals, help plants fight against certain foreign substances.
A phytochemical called lectin may trigger an immune reaction if undigested, resulting in autoimmunity.
Genetic variants can be the root cause of the development of a nightshade allergy.
Mutations in the BCHE gene are associated with nightshade allergy.
The BCHE gene provides instructions for making butyrylcholinesterase (BChE). This cholinergic system enzyme plays a significant role in digestion, blood pressure, heart rate regulation, and spinal cord function.
BChE is a bio-scavenger, essential for:
Low levels of BChE in the body due to mutations may not be sufficient to fight against glycoalkaloids (BChE inhibitors) in nightshades.
Eventually, a nightshade allergy can develop.
Research studies suggest the involvement of specific genes in nightshade allergy.
While nightshade allergies aren't caused by a specific gene, a group of variations in certain genes can have a cumulative effect and increase the risk of allergic reactions.
For example, the BCHE gene plays a role in inactivating the alkaloids present in the nightshade plants.
Any variation in this gene that causes lower levels of poor functioning of the BChE enzyme may result in alkaloid build-up in the body, increasing the risk of a nightshade allergy.
Nightshade allergies are unusual, so you should also consider more common allergens, such as dairy, nuts, seafood, soy, and gluten. Additionally, two factors contribute to nightshade allergies.
Nightshade allergy is mainly caused by the toxic alkaloids in them that defend the plant against molds, pests, and other pathogens.
People develop allergies to alkaloids, which trigger the immune system.
It releases immunoglobulin E (IgE) antibodies to tackle the allergen by releasing histamine into the blood.
This results in nightshade allergy symptoms.
High concentrations of alkaloids like solanine, nicotine, and capsaicin can cause gut irritation and joint inflammation.
People with autoimmune disorders have a weakened immune system.
Weaker immune systems do not respond appropriately to the alkaloids in nightshades, allowing allergies to run rampant.
Rheumatoid arthritis, celiac disease, and inflammatory bowel disease (IBD) are some prevalent autoimmune disorders.
Hand-picked content for you: Could You Have A Wine Allergy? Symptoms, Risk Factors, And More
You are more likely to develop nightshade allergy if you have certain risk factors:
Nightshade allergy is more severe than nightshade intolerance.
While intolerance causes loose stools, bloating, and nausea, which are uncomfortable rather than deadly, allergies can lead to severe symptoms like potentially fatal anaphylaxis.
Initial symptoms can take up to 72 hours to appear, and they can look like:
Similar to other allergies, a doctor can identify a nightshade allergy by performing some diagnostic tests, including:
A standard food allergy treatment involves deleting foods containing the allergen. As instructed by your doctor, keep a food log to track your symptoms and any possible triggers.
Drugs to prevent allergic reactions when exposed may also be part of the treatment approach. Typical prescription drugs include:
EpiPens: Epinephrine injections stop anaphylaxis, a severe allergic reaction that can be fatal.
The simplest method to prevent food allergy symptoms is to avoid the allergens. Here are some easy swaps to common nightshade foods:
| Allergens | Alternatives |
| Tomato sauce | Pesto or Alfredo sauce |
| Tomatoes, | Beetroots, carrots, or grapes |
| Blueberries | Raspberries, strawberries or cranberries |
| Eggplants | Mushrooms |
| Bell peppers | Carrots, onions, celery, or zucchini |
| White potatoes | Sweet potato, radish, or cauliflower |
| Paprika, cayenne, chili flakes | Basil, oregano, black/white pepper |
While onions aren't part of the nightshade family, it's best to stay away from them if you have IBS since they can exacerbate the symptoms.
Interestingly, black and white peppers come from a different family of plants, not from the nightshade family. They're safe to consume if you have a nightshade allergy or intolerance.
Though chocolate isn't a nightshade, it does contain some alkaloids. Fortunately, these are easier to digest than the alkaloids in nightshades, so they shouldn't cause an allergic reaction.
Did you know that Lewy body dementia is 1.5 times more likely to manifest in males rather than females? This condition affects 1.4 million people and their families across the US. If you're wondering what Lewy bodies are, they are clumps of alpha-synuclein protein. They accumulate in the brain, leading to an increasingly severe loss of brain function. Bringing awareness and understanding to this condition can help those affected by Lewy body dementia manage it better. This article will explore the 7 stages of Lewy body dementia and explain everything you need to know about the disease.
Parkinson's patients have Lewy bodies in their brains, too. That's why people who have been diagnosed with Parkinson's can end up with Lewy body dementia.
Read on to learn about the characteristic symptoms of this disease.
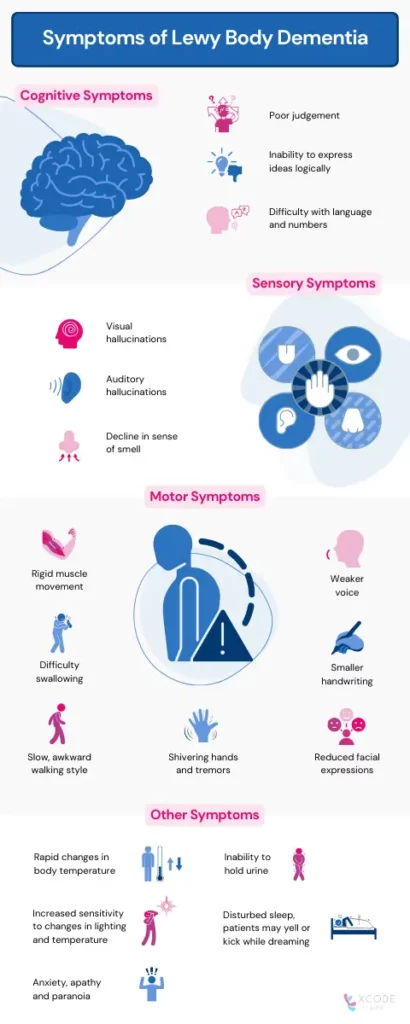
Lewy body dementia limits the capability to think and process information.
The main symptoms present in Lewy body dementia but not in Alzheimer's include:
Most patients experience episodes of delirium, with blank faces and slurred speech.
These phases can last hours or even days.
Patients with Lewy body dementia (LBD) often experience visual hallucinations featuring humans or even animals.
A few patients have even reported hearing and smelling things that aren't there.
Some even say their sense of smell got worse with time.
Difficulty in movement is a common symptom of Parkinson's disease, and this is seen in LBD as well.
They can include:
Subtle signs of the loss of motor function include:
LBD affects the regulation of other organs via the nervous system.
Dysregulated organs could cause:
Understanding how this condition progresses can help afflicted people and their families manage the condition better at each step of this challenging journey.
In this stage, no symptoms are noticeable to the patient or others.
They live life with no interruptions or inconveniences.
Unseen to anyone, proteins begin accumulating in the brain, eventually leading to the formation of Lewy bodies.
Minor instances of forgetfulness begin to take place.
There are rare instances of interruption in day-to-day life and activities.
Since mild lapses in reasoning are also symptoms of aging, it is hard to diagnose at this stage.
In the third stage of the condition, the symptoms become more apparent.
The memory loss worsens, and concentration becomes more difficult for the patient.
Maintaining a schedule becomes harder and harder.
By this time, those around the patient have noticed a decline in brain function and have begun to explore treatment and care options.
The loss of memory begins to take a toll on the patient's near and dear ones. Remembering recent events and even faces becomes a chore at this stage.
Performing day-to-day tasks becomes difficult.
It is at this stage that most patients seek medical intervention and are diagnosed with dementia.
The patient starts to depend on others for bathing and dressing.
Short-term memory loss becomes significant, leading to disorientation and frustration. For now, long-term memories remain preserved.
Significant memory loss accompanies a shift in personality.
At this stage, patients need constant aid to get through all parts of their day, including eating and bathing.
Swallowing and speaking become more difficult due to weaker throat muscles.
A large number of patients lose their ability to communicate verbally.
A handful of patients are no longer able to walk by this stage.
As their physical health worsens, their caregivers focus on comfort and quality of life. The last stage of LBD ends within 1.5 to 2.5 years.
A study published in Elsevier suggests that varied genetic components could lead to LBD.
These genes are related to the working of proteins in the central nervous system.
Mutations in the SNCA and SNCB genes affect neurotransmitter production in the brain, making it harder to think and recall information.
Eventually, misshapen proteins accumulate in the brain, forming Lewy bodies.
It can be hard to diagnose LBD against other neurodegenerative disorders.
The only reliable technique available right now is an autopsy.
Thus, doctors rely on other tests to study brain function.
The one-year rule helps differentiate LBD from other subtypes.
If dementia appears within one year of Parkinson's symptoms, the patient likely has LBD.
Further research into diagnosis through studying blood and cerebrospinal fluid is ongoing.
If successful, LBD could be diagnosed earlier with more accuracy.
There are several medications available to manage the different types of symptoms experienced:
It's important to remember to consult a physician about relevant medication or therapies for your condition.
Although the average life expectancy is 5-8 years after diagnosis, some people have lived up to 20 years with the condition.
Lewy body dementia weakens throat muscles. This deterioration can lead to food or water reaching the lungs, resulting in a fatal case of pneumonia. In most cases, patients succumb to pneumonia or heart failure.
Changes in lighting at dusk can lead to confusion, restlessness, agitation, and distress in patients suffering from Lewy body dementia.
Lewy body dementia - Symptoms and causes - Mayo Clinic
Diagnosing Lewy Body Dementia: For Professionals | National Institute on Aging (nih.gov)
Lewy Body Dementia: Symptoms, Stages, & Treatment (webmd.com)
Dementia with Lewy bodies - Treatment - NHS (www.nhs.uk)
Lewy body dementia - PubMed (nih.gov)
Risk factors for dementia with Lewy bodies - PMC (nih.gov)
Lewy Body Dementia - ScienceDirect
Lewy Body Dementia (LBD) | Johns Hopkins Medicine
Ever worried about catching an ear infection from your child or someone around you? Ear infections, also called acute otitis media, inflames the middle section of the ear, most often in children. The good news is ear infections don't last more than a week and don't need medical intervention. However, without a good understanding of the condition or timely intervention, ear infections can worsen. This article will tell you all you need to know about ear infections and if you should worry about them being contagious.
Ear infections traditionally occur due to microbes, such as bacteria (like Streptococcus) or rhinoviruses, which are responsible for the common cold.
Often, it progresses from another ailment like the flu or an allergic reaction.
Adults exhibit more clear-cut symptoms, such as ear pain and some leakage, but understanding an infant's ear infection can be more complex.
They may show signs like:
Although infective microbes like bacteria and viruses cause ear infections, the infection itself cannot spread from person to person.
What can spread, however, is the existing ailment that led to the ear infection. Infected droplets can easily lead to a cold or the flu.
These conditions then increase the risk of ear infections.
Children are more susceptible to infection since their ears have not fully developed and drain out fluid much slower.
Generally, ear infections caused by viruses heal faster and are gone within a week.
Bacterial infections persist for up to two weeks and can require antibiotic treatment as a doctor may prescribe. They also lead to higher fevers.
Ear infections that respond to antibiotic treatments are bacterial since viruses don’t respond to antibiotics.
Ear infections may not be contagious, but you should remain responsible until they heal.
The internet can suggest thousands of popular home remedies for ear infections, but only a few are credible.
Here are a few things to avoid if you have an ear infection:
Diagnosing an ear infection is relatively easy.
First, doctors check your medical history and perform a physical exam.
Afterward, they can use two main techniques: otoscopy and tympanometry.
An otoscope is a tool that helps a doctor visualize the inside of your ear using a light source.
With a minor modification, a pneumatic otoscope releases a puff of air onto the eardrum.
If the eardrum does not vibrate normally, doctors generally suspect a fluid buildup behind it.
A tympanometer detects changes in pressure in the middle ear.
Understanding this can help doctors gauge how well the middle ear is working.
Sometimes, they can use a tuning fork for this purpose.
Many mild ear infections heal within a few days without treatment.
It may be time to see a doctor if you have:
In such cases, these treatments could help:
Remember to consult your doctor if you show any symptoms. They will guide you correctly.
You can keep ear infections at bay with a few simple strategies:
An infection of the outer ear is known as swimmer's ear or otitis externa.
Research has shown that a mutation in the FUT2 gene slightly alters the composition of the microbes in the ear.
Different microbiota in the ear may affect the chances of ear infection in specific populations worldwide.
According to a 2023 study, a small percentage of headphone users in a study reported hearing loss and ear infection issues. However, the results weren’t conclusive enough to link headphone use to ear infections.
Ear infection (middle ear) - Symptoms & causes - Mayo Clinic
Ear Infection: Symptoms, Causes, Treatment, and More (healthline.com)
Middle-Ear Infection in Adults | Johns Hopkins Medicine
Ear Infection Basics | Ear Infection | CDC
Are Ear Infections Contagious? Here's What to Know (health.com)
Are Ear Infections Contagious? Causes, Treatment, and Prevention (healthline.com)
Swimmer's Ear | Johns Hopkins Medicine
Vicks for Earache: Does It Work and Should You Use It? (healthline.com)
Ear infections - NHS (www.nhs.uk)
Our bodies are happy when our colons are happy. And, how do we keep them happy? Among the many health habits you could adopt, ensuring you get enough fiber tops the list. This is because a lack of fiber in your diet has been associated with a condition called diverticulitis, which occurs when small, bulging pouches develop in your colon and get infected. However, diet is not the only contributor to this condition. A family history of diverticulitis appears to increase one’s risk of developing it, raising a crucial question - is diverticulitis hereditary?
Did you know?
While your DNA can be used to learn about your roots, it can also reveal important things about your gut health. This allows you to take proactive measures for health conditions, even before the symptoms appear, thereby preventing it. You can upload your DNA data to learn 1,500+ things about your health. Learn more.
Diverticula are small bulges or pockets forming in the colon's wall.
They are usually found in the lower part of the colon, called the sigmoid colon, but they can occur anywhere along the colon.
Diverticula are thought to develop due to increased pressure in the colon caused by straining during bowel movements or a low-fiber diet that causes hard stools.
Diverticulitis happens when the diverticula becomes inflamed or infected due to bacteria.
This can happen when fecal matter or food particles get trapped in the diverticula and cause irritation or blockage.
Diverticulitis typically affects older adults, making age a significant factor in its development.
The most frequent symptom of diverticulitis is abdominal pain, usually in the lower left abdomen.
The pain may be sudden, severe, mild, and chronic. It may also radiate to the back or groin.
Other symptoms of diverticulitis may include:
Some people may experience mild or intermittent symptoms of diverticulitis before they develop a full-blown attack.
These early warning signs may include:
You should consult your doctor for further evaluation and treatment if you notice any of these signs.
Early detection and prompt treatment of medical issues can help prevent complications and lower the risk of recurrence.
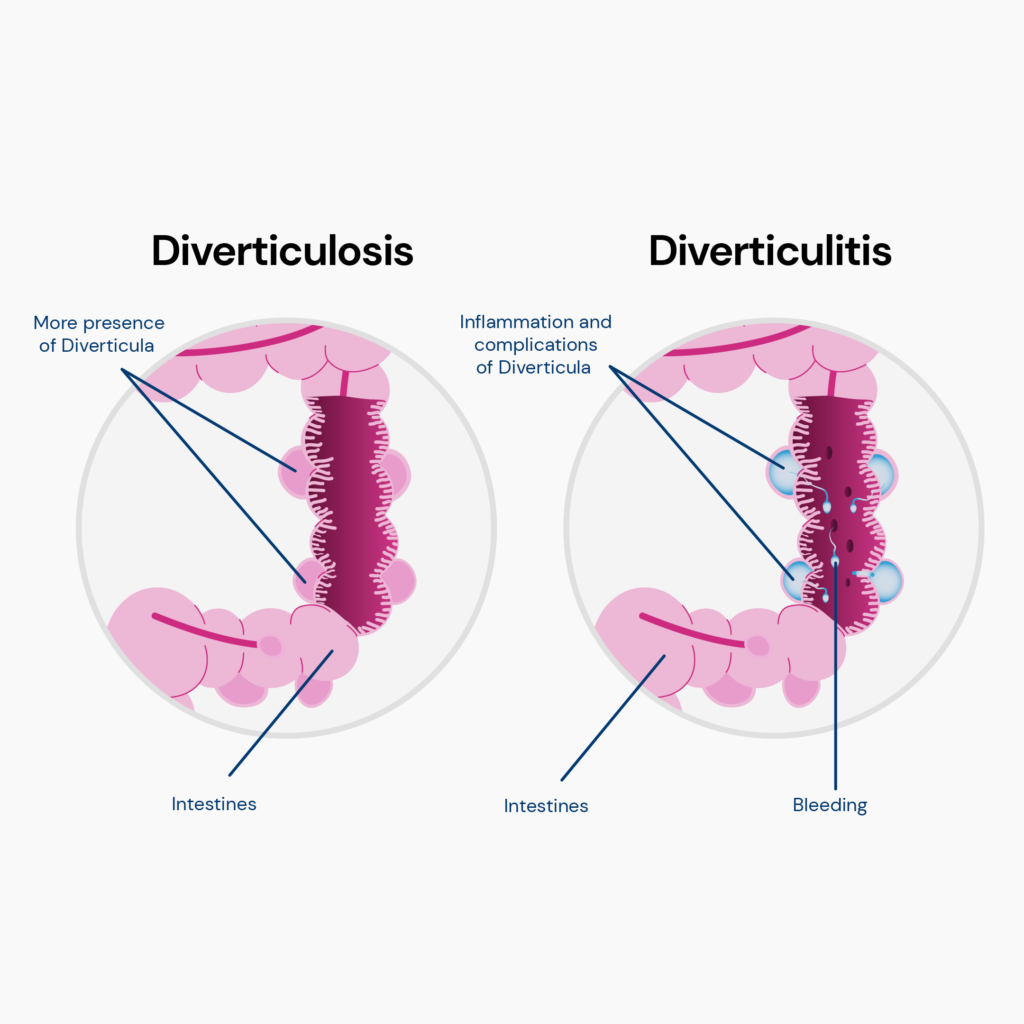
While environmental factors play a significant role in the development of diverticulitis, genetic factors also contribute to its susceptibility and severity.
Research indicates that having a family member with diverticular disease increases your risk of developing the condition.
A study in Denmark analyzed over 142,000 cases of diverticular disease diagnosed in hospitals or outpatient visits.
The findings revealed that the risk of developing diverticular disease is nearly three times higher for siblings of individuals with the condition compared to the general population.
Further evidence comes from a study on twins. It was found that if one identical (monozygotic) twin had diverticular disease, the other twin had a significantly higher chance of having it as well, compared to non-identical (dizygotic) twins.
This suggests a strong genetic component in the susceptibility to diverticular disease.
Moreover, a genome-wide study involving more than 700,000 participants identified 150 genetic factors associated with diverticular disease, underscoring its heritability.
In fact, the study estimated that approximately 40% of the risk for developing diverticular disease is inherited.
These findings collectively suggest that while lifestyle and environmental factors are crucial, genetic predisposition plays a substantial role in the risk and development of diverticulitis.
Diverticulitis is inherited in a complex pattern, which means that a combination of environmental and genetic factors most likely causes it.
However, the exact pattern of inheritance requires further comprehension.
It is unclear whether diverticulitis is inherited in a dominant, recessive, or X-linked manner.
Different genes may also be involved in different cases of diverticulitis.
Researchers have discovered several genes linked to a higher chance of developing diverticulitis.
These genes involve various cellular processes, including inflammation, connective tissue formation, and gut immunity.
It is important to note that even if you have a family history of diverticulitis, it does not mean that you will automatically develop the disease.
Other factors, such as diet and lifestyle, also influence risk.
Variations or changes in several genes act together, each in its own small way, to influence the risk of diverticulitis. Some genes implicated in this condition are:
Remember, these genes alone don't guarantee diverticulitis; environmental factors play a significant role.
The cause of diverticulitis is unknown, but certain risk factors may contribute to its development, such as:
Diverticulitis is typically diagnosed when someone experiences a strong and noticeable attack with severe symptoms.
The diagnosis process can include:
Treatment for diverticulitis depends on how severe it is:
Following certain lifestyle measures can prevent the development of diverticula or reduce the risk of inflammation or infection.
These measures include:
Diverticulitis is a severe condition that can affect your quality of life and lead to complications.
By following these tips, you can prevent or manage diverticulitis and enjoy a healthy and happy colon.

Diverticulitis is when pouches form in the colon wall and become inflamed or infected, often affecting older individuals.
Symptoms include severe abdominal pain, nausea, fever, and bowel changes.
Early signs may include cramps, blood in stool, or feeling incomplete after bowel movements.
While its exact cause is unknown, factors like age, diet, obesity, smoking, and inactivity can contribute.
Studies suggest a family link to diverticulitis. Siblings of those with the condition are three times more likely to get it.
Inheritance is complex, involving genes and environment. Genes like ARHGAP15, COLQ, and FAM155A play roles.
Prevention means a high-fiber diet, hydration, exercise, and quitting smoking.
Genes matter, but lifestyle choices are vital in lowering risk.
Is Diverticulitis Hereditary? Yes, but it's a mix of genes and a way of living.
https://my.clevelandclinic.org/health/diseases/24883-diverticulosis
https://www.health.harvard.edu/blog/looking-out-for-diverticulitis-202108162572
https://www.mayoclinic.org/diseases-conditions/diverticulitis/symptoms-causes/syc-20371758
https://www.sciencedirect.com/science/article/abs/pii/S0016508513000061